Adapted from BMJ Minerva 23 Sept 17 and BMJ Learning Module Clinical Pointers in Diabetic Emergencies Oct 17
Type ones under the age of 30 have a mortality rate three times that of their non- diabetic friends.
This rather shocking statistic was discovered by Welsh paediatricians who have been tracking their children with diabetes since 1995. Furthermore the death rate has not gone down over all this time despite improvements in monitoring and therapy. Ketoacidosis is the leading cause of death. Although microvascular and to a lesser extent macrovascular complications can occur, they do not affect mortality rates in this age group.
Out of a hundred or so type one adult diabetics approximately 3 or 4 will develop diabetic ketoacidosis each year. Currently 3-5% will die. Not all deaths will occur in hospital because not everyone is identified as having ketoacidosis prior to death. Recognition by relatives, friends, police and medical professionals would be an important factor to improve transfer to hospital.
Ketoacidosis is also be the presenting sign of diabetes in 6% of the total number of ketoacidosis patients. It may have been precipitated by a viral infection and can be confused by a variety of illnesses such as gastroenteritis, flu and alcohol intoxication and withdrawal.
Assuming a person can be recognised as ill and needing hospital assessment, recognition of DKA is improved by always checking a blood glucose in an acutely ill person in the A and E department.
If levels of glucose are high, and the characteristic symptoms are present eg dehydrated looking, tired, nausea, vomiting, abdominal discomfort and breathing rapidly, then the diagnosis can be further explored by checking the blood electrolytes.
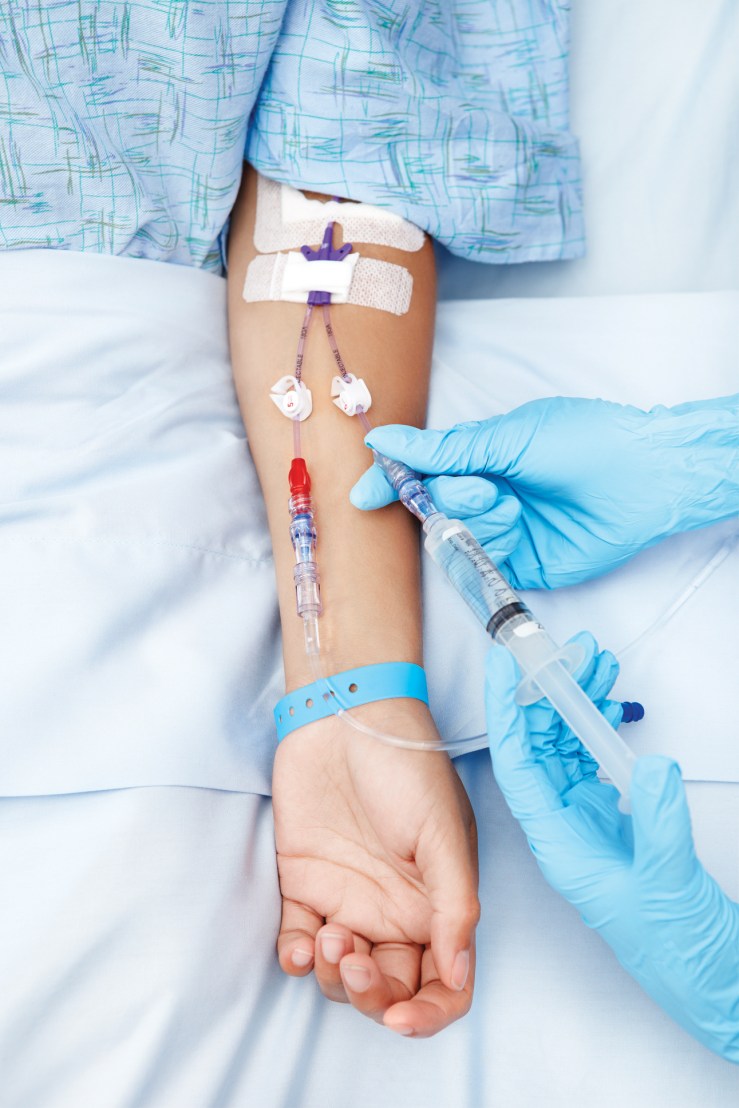
The immediate treatment is re-hydration with a litre of normal saline and the administration of intravenous or subcutaneous insulin usually 0.1 u of insulin per kilogram body weight. As the potassium level can be affected, particularly a tendency to go too low after treatment has started to work, this needs monitored every hour or two. The problem is that irregularities of the heart beat can occur if the potassium level is not adjusted correctly.
It can be seen that management of DKA in the established case is tricky and time consuming. Therefore it is wise to seek medical advice while you or the one you are concerned about, is still relatively well and can for instance still tolerate oral fluids and give a coherent history.
Early recognition and treatment is the key to a good outcome in DKA.

I think we are so concerned with lows that we often forget the long and short run impact oh high blood sugar. I know I am ancient when it comes to diabetes management, but I was taught to deal with the lows and avoid the highs. Many parents at a school i worked at were preoccupied with lows and seldom worried about highs. Its a balance and both are dangerous.
LikeLiked by 1 person
Interesting point, Rick – especially that you’ve seen people diagnosed in the years after you more worried about lows than highs. That says a great deal about the changing nature of diabetic education. As someone diagnosed in the early 80s, I’m sure the emphasis was on avoiding the highs, though I’d need to check with my mum as she’d remember better than I.
LikeLike
I have had DKA at least twice and maybe a third time. Stupid mistakes of my own making except the first. When I became a diabetic back in 1977 it was treated as you talked about. What I did not know until years later was that one of the doctors stayed at the hospital over night in case something else went wrong. They were not sure I would survive the night. Never a comforting thought. I find myself in a tight spot. I am so sensitive to insulin, especially for someone who has had it this long and who is 48 years old. My history of being so combative when low has made me fear hurting someone much more than any damage I may do to myself so I run it higher. I try to keep it under 200 (11.1) but I don’t get too excited if it gets higher. Just last night it was 391 so I corrected at breakfast before going to work overnight. By 1:30 am it was down to 67 and still dropping. Worked harder than I had planned I guess. In my world, although I fear them both, the lows scare me more.
LikeLike
Hey Bob, that’s tough – that super sensitivity. I find the same thing – fast-acting insulin often acts like a sledge hammer on me, and it feels most unpleasant. I find exercise, low-carbing and fasting helpful, but realise that’s not for everyone. Best wishes, Emma
LikeLike