 The Society for Vascular Surgery, the American Podiatric Medical Association and the Society for Vascular Medicine collaboratively publish first-ever set of clinical practice guidelines for treating the diabetic foot. These took three years to develop and are available online.
The Society for Vascular Surgery, the American Podiatric Medical Association and the Society for Vascular Medicine collaboratively publish first-ever set of clinical practice guidelines for treating the diabetic foot. These took three years to develop and are available online.
Specific areas of focus included (1) prevention of diabetic foot ulceration, (2) off-loading, (3) diagnosis of osteomyelitis, (4) wound care, and (5) peripheral arterial disease.
They include preventive recommendations such as those for adequate glycemic control, periodic foot inspection, and patient and family education.
They recommend using custom therapeutic footwear in high-risk diabetic patients, including those with significant neuropathy, foot deformities, or previous amputation. In patients with plantar diabetic foot ulcer (DFU), they recommend off-loading with a total contact cast or irremovable fixed ankle walking boot.
In patients with a new DFU, they recommend probe to bone test and plain films to be followed by magnetic resonance imaging if a soft tissue abscess or osteomyelitis is suspected.
They provide recommendations on comprehensive wound care and various débridement methods. For DFUs that fail to improve (>50% wound area reduction) after a minimum of 4 weeks of standard wound therapy, they recommend adjunctive wound therapy options.
In patients with DFU who have peripheral arterial disease, they recommend revascularization by either surgical bypass or endovascular therapy.
Whereas these guidelines have addressed five key areas in the care of DFUs, they do not cover all the aspects of this complex condition. Going forward as future evidence accumulates, they plan to update recommendations accordingly.
Diabetes is one of the leading causes of chronic disease and limb loss worldwide, currently affecting 382 million people. It is predicted that by 2035, the number of reported diabetes cases will soar to 592 million. This disease affects the developing countries disproportionately as >80% of diabetes deaths occur in low- and middle-income countries.
As the number of people with diabetes is increasing globally, its consequences are worsening. The World Health Organization projects that diabetes will be the seventh leading cause of death in 2030. A further effect of the explosive growth in diabetes worldwide is that it has become one of the leading causes of limb loss. Every year, >1 million people with diabetes suffer limb loss as a result of diabetes. This means that every 20 seconds an amputation occurs in the world as an outcome of this debilitating disease. Diabetic foot disease is common, and its incidence will only increase as the population ages and the obesity epidemic continues.
Approximately 80% of diabetes-related lower extremity amputations are preceded by a foot ulcer. The patient demographics related to diabetic foot ulceration are typical for patients with long-standing diabetes. Risk factors for ulceration include neuropathy, PAD, foot deformity, limited ankle range of motion, high plantar foot pressures, minor trauma, previous ulceration or amputation, and visual impairment. Once an ulcer has developed, infection and PAD are the major factors contributing to subsequent amputation.
Available U.S. data suggest that the incidence of amputation in persons with diabetes has recently decreased; toe, foot, and below-knee amputation declined from 3.2, 1.1, and 2.1 per 1,000 diabetics, respectively, in 1993 to 1.8, 0.5, and 0.9 per 1,000 in 2009. However, including the costs of outpatient ulcer care, the annual cost of diabetic foot disease in the United States has been estimated to be at least $6 billion. A Markov modeling approach suggests that a combination of intensive glycemic control and optimal foot care is cost-effective and may even be cost-saving.
DFUs and their consequences represent a major personal tragedy for the person experiencing the ulcer and his or her family as well as a considerable financial burden on the healthcare system and society. At least one-quarter of these ulcers will not heal, and up to 28% may result in some form of amputation. Therefore, establishing diabetic foot care guidelines is crucial to ensure the most cost-effective healthcare expenditure. These guidelines need to be goal focused and properly implemented.
This progression from foot ulcer to amputation leads to several possible steps where intervention based on evidence-based guidelines may prevent major amputation. Considering the disease burden and the existing variations in care that make decision-making very challenging for patients and clinicians, the SVS, American Podiatric Medical Association, and Society for Vascular Medicine deemed the management of DFU a priority topic for clinical practice guideline development. These recommendations are meant to pertain to all people with diabetes regardless of etiology.
Practice Pearls:
•“The Management of the Diabetic Foot,” was developed after three years of studies and later published online and in print in the Journal for Vascular Surgery.
•This progression from foot ulcer to amputation lends to several possible steps where intervention based on evidence-based guidelines may prevent major amputation.
•Every year, >1 million people with diabetes suffer limb loss as a result of diabetes.
Researched and prepared by Steve Freed, BPharm, Diabetes Educator, Publisher and reviewed by Dave Joffe, BSPharm, CDE
Anil Hingorani, MD Glenn M. LaMuraglia, MD, Journal of Vascular Surgery Feb 2016 , Volume 63, Issue 2, Supplement, Pages 3S–21S
April 23rd, 2016 Diabetes in Control
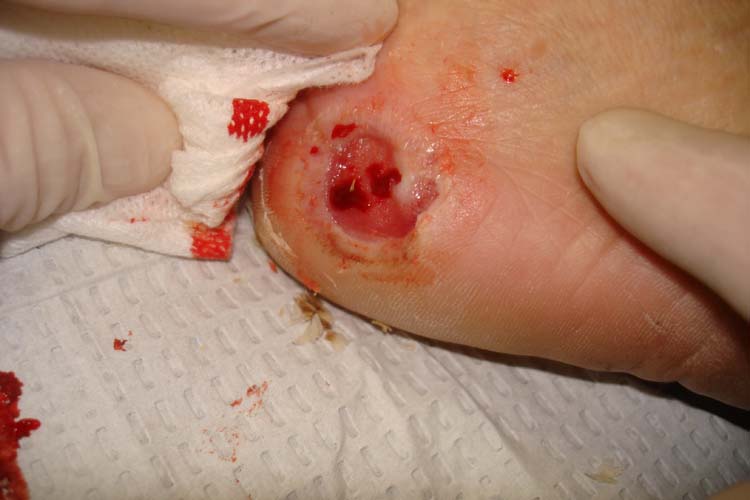
Having seen what diabetes can do with feet, I for one am glad for any increased treatment guidelines
I referred your article to the TUDiabetes.org blog page for the week of August 8, 2016.
LikeLike