In part 1, I have discussed the use of ‘healthy’ and ‘all natural’ statements on the food labels. Now I will talk about the labels that claim low or no fat or sugar.
3. No Sugar Added.
This sounds rather confusing, because it prompts you to think that the product contains no sugar at all. If you have diabetes, you might want to buy it for this very reason. Now wait a minute.
“No sugar added” doesn’t mean that the product is carb-free or calorie-free. It is sometimes being confused with sugar-free; in fact, there’s a bunch of websites that do just that. The problem is that some foods have sugar in them naturally, such as for example, milk or fruit, so anything containing these two can’t be sugar-free. Besides, no sugar added products can still contain additives with high glycemic index such as Maltodextrin.
 Maltodextrin is made of corn, rice, potato starch, or wheat; it’s a common food additive used for expanding the volume of processed food and for increasing its shelf life.
Maltodextrin is made of corn, rice, potato starch, or wheat; it’s a common food additive used for expanding the volume of processed food and for increasing its shelf life.
It has 4 calories per gram which is the same as table sugar. However, maltodextrin has a high glycemic index, almost twice as much as table sugar does. GI of maltodextrin is 110, compared to 65 of table sugar. This means that it can raise the blood sugar levels very quickly. Per FDA, Maltodextrin has to be listed in the nutrition panel as what it is, a carbohydrate.
4. Sugar-free
This doesn’t automatically mean fewer calories; in fact, sugar-free products still have some sugar in them. By FDA definition, sugar-free foods can have less than 0.5 grams of sugar per serving. They however still have calories and carbs from other sources. One of such sources are sugar alcohols that taste just as sweet as sugar while having half the calories.
Most sugar alcohols have no effect on blood sugar. Some of them however are actually carbohydrates that are well absorbed by the body and can cause blood sugar spikes such as Maltitol. Sugar alcohols can also act as a laxative so keep that in mind when indulging.
Sugar-free products can also have artificial sweeteners that don’t affect blood sugar directly but can affect insulin sensitivity nevertheless.
When I was first diagnosed with diabetes, I started buying sugar-free products thinking that I was doing the right thing. One of the first such products was sugar-free pancake syrup that tasted as sweet as its sugar-containing counterpart. For a brief while I was proud of myself for being able to find a product that is sugar-free and just as sweet. This however was short lived when I had a seemingly unexplained blood sugar spike after eating hot cereal with ‘sugar-free’ syrup. I then took a close look at the Nutrition Panel and low and behold, it listed a few carbs including Sorbitol, a sugar alcohol; corn syrup and molasses. All of the above are carbs.
After having contacted my nutritionist, I was advised to stay away from everything that ends with ‘ol’ (sugar alcohols). From now on, I will never take the statement ‘sugar-free’ for granted but will read the labels first and then decide. A lesson learned.
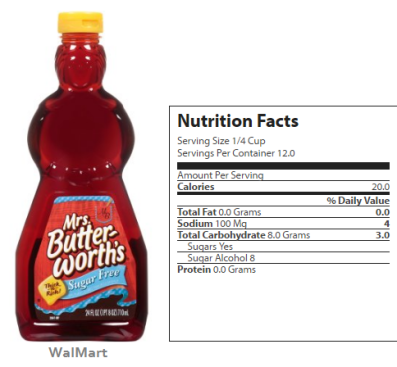

Here now, a bottle of pancake syrup; didn’t the label say “sugar-free”? Yes, it did but the Nutrition Facts panel states Sugars – Yes, and the amount of 8 grams. This is per serving size that mind you, is a quarter of a cup.
Most if not all of us consume a few times over this in one sitting. No, really. A quarter of a cup is a little bitty thing. Most folks will use at least a cupful of it. Then all the seemingly ‘healthy’ content goes out the window.
Ever seen a commercial with a pile of pancakes buried under a huge mound of syrup? There goes your serving size.
5. Low-fat or fat-free
Many of us associate zero trans fat or fat-free claims with healthy, which is exactly the outcome the food manufacturers are trying to achieve. And the truth is, while some foods are naturally low in fat, such as fruits and vegetables, processed food is another story. Fat-free versions of food replace fat with sugar which is no better and eventually gets stored in your body as fat anyway. The keywords to look for are corn syrup and fructose.
Fat-free products are loaded with sugar, and sugar-free are loaded with fat. Here you have it, a no-win situation.
Nutritionpedia website has posted these two labels side-by-side, one is regular, the other, fat-free.

As you can see, the fat-free product contains about three-fold more sugar than the regular version of the same product. Not only would one serving size of the fat-free food have more calories than the full-fat version but you may be tempted to eat two servings because it comes across as healthy.
By FDA standards, low fat means less than 3 grams of fat per serving size and fat-free, less than 0.5 grams. How much is the serving size? This is what the food manufacturers are playing with. One vs two cookies as a serving size or slices of bread likewise, can make all the difference. And who is eating only one cookie? When you or your kids eat more than one, all that low fat content per serving size goes out the window.
THE BOTTOM LINE: sugar-free products are loaded with fat, and fat-free, with sugar. To make sure that you are in fact eating healthy food, you need to do your homework. Check the label of a fat-free or sugar-free product and compare it with the full-fat or full-sugar version. This of course will take some time.











 Feature
Feature

 We know about the issue of slowed metabolism after weight loss due to the lean muscle mass loss that goes along with fat loss. This is one reason why higher protein/low carb diets work better than low fat diets; because muscle mass is maintained better. Well, new information from Diabetes in Control backs up what some of us know intuitively or may have experienced personally….
We know about the issue of slowed metabolism after weight loss due to the lean muscle mass loss that goes along with fat loss. This is one reason why higher protein/low carb diets work better than low fat diets; because muscle mass is maintained better. Well, new information from Diabetes in Control backs up what some of us know intuitively or may have experienced personally….



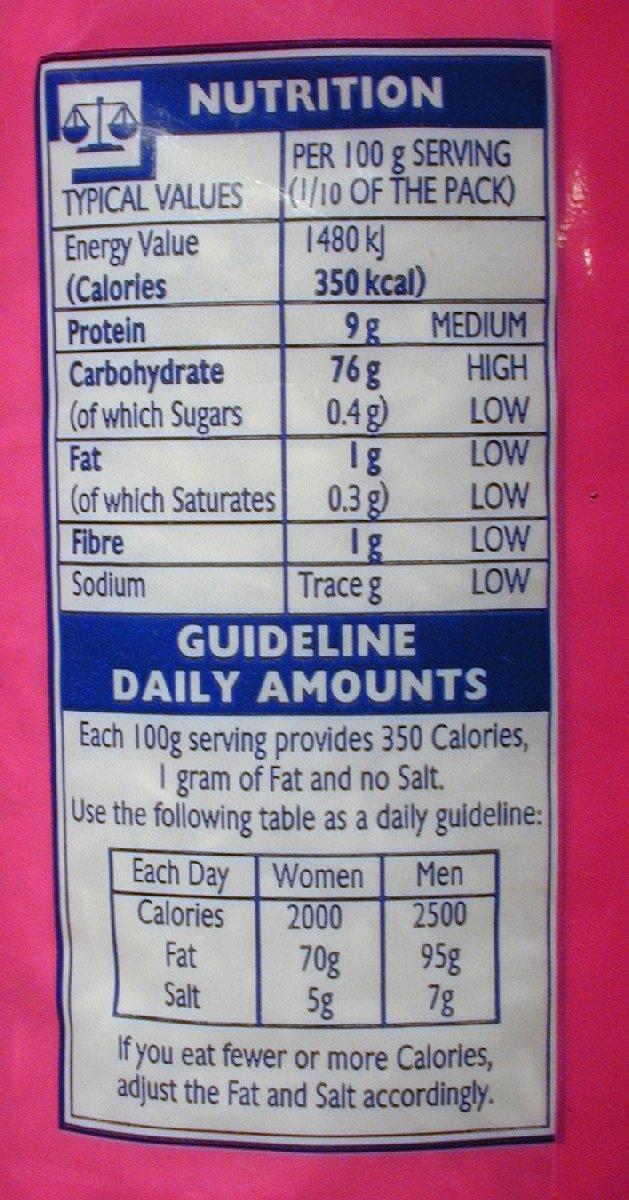



 Maltodextrin is made of corn, rice, potato starch, or wheat; it’s a common food additive used for expanding the volume of processed food and for increasing its shelf life.
Maltodextrin is made of corn, rice, potato starch, or wheat; it’s a common food additive used for expanding the volume of processed food and for increasing its shelf life.


I’m delighted that The BMJ has stood by this article and decided against retraction. Two outside reviewers judged that the criticisms of the piece did not merit its retraction, and in the end, the corrections made by The BMJ do not, in my view, materially undermine any of the article’s key claims. This article therefore stands as one of the most serious ever, peer-reviewed critiques of the expert report for the US Dietary Guidelines for Americans (DGAs).
The importance of the DGAs, and therefore of this article, should not be understated (and indeed was recognized by many in the mainstream media when the article was published). The DGAs have long been considered the “gold standard,” informing the US food supply, military rations, US government feeding assistance programs such as the National School Lunch Program which are, altogether, consumed by 1 in 4 Americans each month, as well as the guidelines of professional societies and governments around the world, and eating habits generally.
Yet rates of obesity began to shoot upwards in the very year, 1980, that the DGAs were introduced, and the diabetes epidemic began soon thereafter. A critically important yet little understood issue is why the DGAs have failed, so spectacularly, to safeguard health from the very nutrition-related diseases that they were supposed to prevent.
In documenting fundamental failures in the science behind the DGAs, this article offers new insights; It establishes that a vast amount of nutrition science funded by the National Institutes of Health and other governments worldwide has, for decades, been systematically ignored or dismissed, and that therefore, that the DGAs are not based on a comprehensive reviews of the most rigorous science. Incorporating this long-ignored relevant science would likely lead to fundamentally different DGAs and could very well be an important step in infusing them with the power to better fight the nutrition-related diseases.
A fundamental question is why 170+ researchers (including all the 2015 DGA committee members, or “DGAC”), organized by the advocacy group, the Center for Science in the Public Interest (CSPI), would sign a letter asking for retraction. After all, in the weeks following publication, any person had the opportunity to submit a “Rapid Response” to the article, and both CSPI and the DGAC did so, alleging many errors. I responded to them all in my Rapid Response. This is the normal post-publication process.
Yet after all this, CSPI returned for a second round of criticisms, recycling two of the issues (CSPI points #3 and #10) that I had already addressed in my Rapid Response (and which had required no correction), adding another 9 (one of which, #4, contained no challenge of fact), and demanding that based on these alleged errors, the article be retracted. CSPI then circulated this letter widely to colleagues and asked them to sign on.
This lack of substance in the retraction effort seems to point to the reality that it was first and foremost an act of advocacy—a heavy handed attempt to silence arguments with which CSPI, a longtime supporter of the Dietary Guidelines and its allies disagree.[ footnote 1] And this applies not just to the retraction letter but to other CSPI efforts to stifle alternative viewpoints. Earlier this year, for example, I was dis-invited from the National Food Policy Conference after CSPI, together with the USDA official in charge of the Dietary Guidelines, threatened to withdraw if I were included, details of which are reported here and which a Spiked columnist called an act of “censorship.”
It’s important to note that I am not the only person disturbed by the lack of rigorous science underpinning our dietary guidelines. Numerous scientists around the world have expressed concern about the science. And indeed, this consternation is shared by no less than the US Congress, which held a hearing on Oct 7, 2015 to address its serious doubts about the DGAs. Such was this concern that last year that Congress mandated the first-ever major peer-review of the DGAs, by the National Academy of Medicine. Congress appropriated $1 million for this review, and it additionally stipulated that all members of the 2015 DGA committee recuse themselves from the process.
What is the dangerous information challenging the DGAs that cannot be heard on a conference panel nor published in a peer-reviewed journal?
The major findings of this article are that:
1. The DGAC’s finding that the evidence of a “strong” link between saturated fats and heart disease was not clearly supported by the evidence cited. (Note that as of last year, the Heart and Stroke Foundation of Canada no longer limits saturated fats. Note, also, that Frank Hu, the Harvard epidemiologist in charge of the DGAC review on saturated fats, was an energetic promoter of the retraction letter against my article that critiqued his review, according to emails obtained through FOIA requests);
2. Successive DGA committees have for decades ignored or dismissed a large body of rigorous (randomized controlled trial) literature on the low-fat diet, on more than 50K subjects, collectively finding that this diet is ineffective for fighting obesity, diabetes, heart disease or any kind of cancer;
3. Although the DGAs have for decades recommended avoiding saturated fats and cholesterol to prevent heart disease, no DGA committee has ever directly reviewed the enormous body of rigorous (government-funded, randomized controlled trials) evidence, testing more than 25,000 people, on this hypothesis. Many reviews of this data have concluded that saturated fats have no effect on cardiovascular mortality;
4. The DGAC ignored a large body of scientific literature on low-carbohydrate diets (including several “long term” trials, of 2-years duration) demonstrating that these diets are safe and highly effective for combatting obesity, diabetes, and heart disease;
5. The Nutrition Evidence Library (NEL) set up by USDA to do systematic reviews of the science did not meet its own standards for its review of saturated fats in 2010;
6. Although the DGAC is supposed to consult the NEL to conduct systematic reviews of the science, the 2015 DGAC did so for only 67% of the questions that required systematic reviews;
7. For a number of key reviews, the 2015 DGAC relied on work done in part by the American Heart Association and the American College of Cardiology, which are private associations supported by industry and therefore have a potential conflict of interest;
8. The DGAs, for the first time, introduce the “vegetarian diet” as one of its three, recommended “Dietary Patterns,” yet a NEL review of this diet concluded that the evidence for this its disease-fighting powers is only “limited,” which is the lowest rank of evidence assigned for available data;
9. The DGA’s three recommended “Dietary Patterns” are supported by only limited evidence. The NEL review found only “limited” or “insufficient” evidence that the diets could combat diabetes and only “moderate” evidence that the diets can help people lose weight. The report also gave a strong rating to the evidence that its recommended diets can fight heart disease, yet here, several studies are presented, but none unambiguously supports this claim. In conclusion, the quantity of recommended diets are supported by a small quantity of rigorous evidence that only marginally supports claims that these diets can promote better health than alternatives;
10. The DGA process does not require committee members to disclose conflicts of interest and also that, for the first time, the committee chair came not from a university but from industry;
11. The 2015 DGAC conducted a number of reviews in ways that were not systematic. This allowed for the potential introduction of bias (e.g., cherry picking of the evidence).
This last claim, on the systematic nature of the DGAC reviews, is the subject of the corrections published in The BMJ this week, and refer to CSPI points #1, #2, #7, and #8 (two of which are statements in the text and two of which are in the supporting tables). I am grateful to have had the opportunity to work with The BMJ on developing this notice.
The BMJ has placed a word limit on my response. For the rest of this comment, please see: http://thebigfatsurprise.com/comment-bmj-correction-notice/
Footnote 1
CSPI has fought for decades to eliminate saturated fats from the American food supply (so much so, that throughout the late 1980s, CSPI advocated for replacing saturated fats with trans fats and succeeded in driving up consumption of trans fats to historic levels, as described in The Big Fat Surprise, pp.227-228). CSPI has also long advocated for shifting away from animal foods containing saturated fats, towards a plant-based diet based on grains and industrial vegetable oils. The researchers who joined CSPI in signing the letter are largely adherents to this view; many have participated in generating the science that has been used to support the hypothesis that fat and cholesterol cause heart disease, and it is upon this hypothesis that the Guidelines have been based.
Competing interests: I have read and understood BMJ policy on declaration of interests and declare that I am the author of The Big Fat Surprise (Simon & Schuster, 2014), on the history, science, and politics of dietary fat recommendations. I have received modest honorariums for presenting my research findings presented in the book to a variety of groups related to the medical, restaurant, financial, meat, and dairy industries. I am also a board member of a non-profit organization, the Nutrition Coalition, dedicated to ensuring that nutrition policy is based on rigorous science.