 Diabetic foot ulcers that don’t respond to usual care can respond very well to a new membranous patch that is available to patients in the USA.
Diabetic foot ulcers that don’t respond to usual care can respond very well to a new membranous patch that is available to patients in the USA.
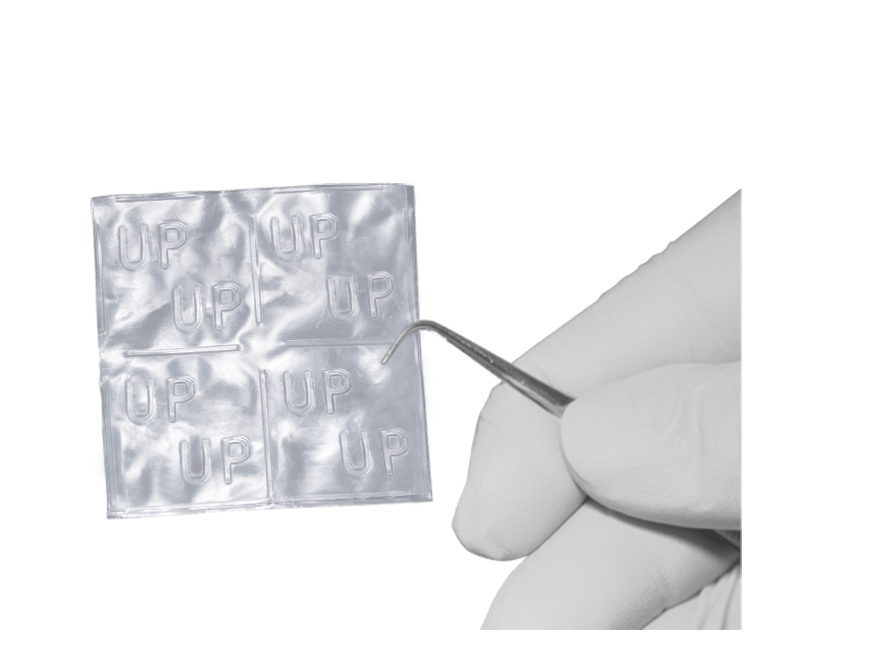
Dr Dan Fetterolf, head physician at the MiMedx Corporation, gave an interview to Diabetes in Control this month and described how this treatment fits into therapy for foot ulcers. The Epifix patches are derived from the amniotic membranes of women who have been screened for blood borne viruses and who are to be delivered by caesarean section. At delivery the placenta is put in a sterile container and sent to the USA production site.

Diabetic foot ulcers are bad news for patients. In the USA the cost of ulcer treatment or amputation has to be borne between the patient and health maintenance organisation. Thus there tends to be more interest in preventative treatments even when these are expensive. When an ulcer has not responded to the usual debridement, moist dressings and anti-microbial efforts after a month, these ulcers have a relatively poor prognosis and the use of amniotic membrane treatments make financial good sense.
Diabetics have a lifetime risk of getting a foot ulcer of 25%. Around a fifth of these people will go onto having an amputation. Many of these will have additional factors that increase the risk such as neuropathy that prevents people from feeling trauma to the feet, peripheral vascular disease that delays healing and obesity that adds to the pressure on the feet. Once an amputation occurs that person’s life expectation reduces and their ability to earn decreases. They need much more in the way of social and medical support. These factors all affect the person’s family as well as the economy of the countries concerned.
Prevention of diabetic foot ulcers involves good glycaemic control, daily shoe and foot examination by the person with diabetes and regular foot examination and testing by health care professionals. If an ulcer does develop then tighter adherence to preventative measures becomes essential. Weekly follow up of patients is required.
To allow maximal healing it is important to offload weight on the affected foot as much as possible. Dressings should not be allowed to dry out or else the layer of protective epithelium can be removed at the same time the dry dressing comes off.
Chronic ulcers come with a whole collection of adverse healing factors. Most people will have neuropathy and at least a degree of peripheral vascular disease. The healing ability of the skin is reduced as inflammatory cytokines reduce the healing process. In addition the immune system is rendered less effective by the glycation of immunoglobulins and other factors.
Diabetes now affects 7-10% of the USA population and in certain countries it is higher. The Pima Indians have worldwide the highest proportion of adult diabetes at 50% partly due to genetics and partly due to their very high sugared drinks ingestion. In the affluent areas of the Middle -East such as Dubai and Saudi Arabia levels are also very high. There is a genetic issue here but also a very high sugar intake. Scotland is remarkably dreadful too. A lot of this is due to deprivation and our characteristically poor diet. Many families eat no fruit and vegetables at all. Well, if we can’t beat England at football, we can certainly be winners when it comes to obesity- diabetes prevalence.
From our point of view on diabetesdietblog.com we welcome a strategic approach to reducing the number of people who develop diabetes, and improving the outlook for those who do develop the condition. Proper dietary education and provision in the public domain are essential. Only by doing this can glycaemic control be tackled in a robust manner. When a patient does develop an ulcer, resources to heal this effectively and reduce the progression to amputation is key. If this new treatment could become available in the UK it would be very much welcomed as a way to improve patient’s lives as well as cut back the nursing and medical costs associated with the prolonged treatment of ulcers.

 Dr Brian Wansink is a behavioural economist who studies people’s behaviour around food. Specifically he is interested in how the environment can be manipulated to support or sabotage weight loss efforts. In an interview for Diabetes in Control at the ADA conference in 2012 he outlined the five areas in which we tend to eat more than we intend.
Dr Brian Wansink is a behavioural economist who studies people’s behaviour around food. Specifically he is interested in how the environment can be manipulated to support or sabotage weight loss efforts. In an interview for Diabetes in Control at the ADA conference in 2012 he outlined the five areas in which we tend to eat more than we intend.
 In the UK 25% of adults are obese, the highest prevalence in Europe, and type 2 diabetes has risen by 65% in the past 10 years with no sign of slowing down. Together they cost the NHS £16 billion a year and the UK economy at large £47 billion a year.
In the UK 25% of adults are obese, the highest prevalence in Europe, and type 2 diabetes has risen by 65% in the past 10 years with no sign of slowing down. Together they cost the NHS £16 billion a year and the UK economy at large £47 billion a year.











