When Nick Jonas was 13, he was diagnosed with Type 1 diabetes, and his life was never the same. He describes it as a time of confusion, fear and unknowing.
Category: health
Heri’s health points: Great meal planning app for all sorts of food plans

This was my typical work day a year ago:
- Grab a bowl of cereal or whatever there is in the fridge for breakfast.
- Run to the subway and grab a coffee on my way to work.
- A bagel with cream cheese, a shawarma, a muffin or whatever I could find at lunch. This would coincide with my third cup of coffee of the day. Other times, I went to a restaurant for a business meeting and this would be my main meal of the day.
- Go to a networking evening event and eat whatever they have. Pretzels, beers, coffee, chips, you name it. If there is no event, I would otherwise pick up a hefty meal from a neighboring restaurant on my way home.
Repeat this five days a week and you have a recipe for disaster. It is a diet composed of processed foods, refined carbs and inflammatory foods that lead to obesity, Type 2 Diabetes, or worse.
The sad state of affairs prompted me to get Mealime, a free app available on Android and iPhone. It is also available on the web, but this 9 months review only covers the mobile app.
I find Mealime is an excellent meal and nutrition planner. Akin to having a training plan, meal planning allows you to have consistent nutrition that you can easily track, and improve later on. This is good for those with serious athletic goals, who want to have good health or those who have chronic diseases.
Without meal planning, you are more likely to improvise, eat out, and deviate from health goals. It also makes food tracking difficult. Who would wish to list all ingredients in their food if every meal was different? No one.
How it works
Mealime asks for your food preferences on setup. Classics is for most people. Low Carb means limited glucides and instead more healthy fats. Vegetarian is zero meat. There is also Paleo, Pesceterian and Flexitarian, options I didn’t know about.
My goal was to control blood sugar and insulin levels so I chose low carb.

Mealime also asks for allergies and ingredients you dislike. I dislike for example turnips.
After choosing a menu type, it then asks you how many meals you wish to prepare.

If you don’t like a dish, you can swipe left, until you have all the meals you want.
The app then shows a summary of ingredients. I find this very practical when doing groceries.

You know exactly what to get and what not to get. This reduces my stress, and I feel like a master chef
Hey, we are cooking!
Prior to Mealime, my cooking skills were limited to basic omelettes or making batches of kitchen breasts. Naturally, I was apprehensive. Disaster, anyone?
I was positively surprised to find that Mealime dishes are not difficult to make. They take on average 40 minutes to make and never require any special talent or instruments. It takes a good knife, a pan and an oven. And a smile
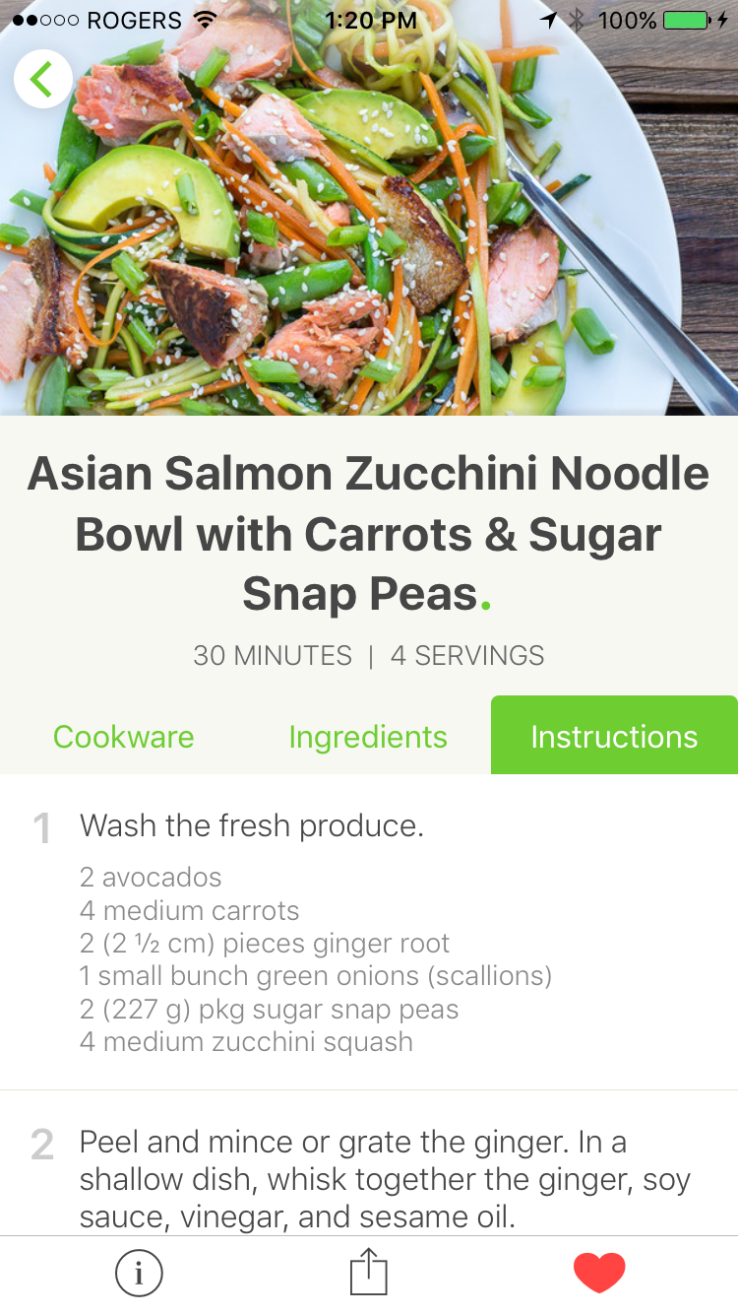
Since then, I changed to a better chef’s knife, a good skillet and more spices but you can always manage with what you have at home.
Easy Meal Planning for the week
I do groceries on weekends, then cook a Mealime dish in the evening. I have a delicious dinner and put the rest in containers. They usually last 3 days, and usually I cook again mid-week.
If we take the baseline of 40 minutes for meal preparation, that means every dish takes me 40 / 7 ~ 6 minutes to make. Surely beats going to a take-out restaurant!
If you favorite a dish, it is always available through a shortcut. For instance, I often make wild atlantic salmon with zucchini and carrots. You can then add the recipe in MyFitnessPal, which means food tracking takes only a few seconds. It’s a nice streamlined process to take control of your nutrition intake.
Dramatic Results
By following the low carb option, and commuting by bike, I lost a lot of weight in a few months (~7kgs). The loss was dramatic and many friends and acquittances could not believe it.
The biggest benefit I find however is great overall energy, eating more vegetables, and learning to appreciate good food cooked at home. This is a life skill I underestimated previously and I am glad Mealime helped.
It also makes my life easy, and lets me invest my time elsewhere.
A Perfect App?
I have not used other food apps so I can’t say on how it compares to other competitors. I can say however Mealime is great for those with limited time and want to cook healthy meals. It provides nutritious fuel for my running and daily work and can wholly recommend it. Download it and give it a go !
Sky: How you can respond sensitively when a friend gives you devastating news
10 Amazing Reactions to Bad News: The Right Way to Respond to a Friend’s Hardship – By Sky Khan – Kindness Blog
10 Amazing Reactions to Bad News: The Right Way to Respond to a Friend’s Hardship – By Sky Khan
What to Say to Someone with Cancer
It’s hard to know what to say to someone with cancer. If you’re like most, you blurt an instinctive, “I’m sorry.” Albeit well-intentioned, “I’m sorry” is a sorry substitute for a meaningful connection during a vulnerable time.

Sky Khan knows how to react when receiving bad news. She became an involuntary, repeated “bad news teller” after doctors diagnosed her 4-year-old daughter, Kiki, with leukemia last September.
After hours of face-to-face conversations and challenging phone calls, Sky heard and saw reactions across a spectrum of appropriateness. These firsthand experiences motivated her to reflect on what to say to someone with cancer or facing any sort of life challenge.
Sky compiled her insights into this list to help others. You can read more about Sky, Kiki, and their family by visiting Kiki’s Leukemia Battle Fund.
10 Amazing Reactions to Bad News: The Right Way to Respond to a Friend’s Hardship
Here’s a list of the top 10 things my friends said or did that provided comfort, reassurance, and warmed me to the core. The next time you find yourself reacting to someone’s bad news, have a few responses from this list ready to go and you won’t be left stumbling for the right thing to say or do.
1. Thank you so much for telling me.
A simple thank you was one of the most surprisingly sweet reactions that I received. When a friend felt that it was a privilege to receive my news, it meant so much. Thank you, along with an attentive, calm presence, provided a very comforting result. Sometimes all that’s required in a difficult situation is being a witness to someone else’s anxiety or sorrow. If you only have a few words to offer, saying thank you is a nice alternative to the overdone, ‘I’m sorry’.
2. This really puts things in perspective.
When I was able to provide a friend with the opportunity to reflect on his own health and well-being, it brought optimism to the conversation. It also allowed space to take the focus off of my daughter’s situation, which was often a welcome relief. When a friend was able to express both compassion and a sense of gratitude, the conversation turned hopeful. It is not always easy to appreciate good health while you have it.
3. I’m coming over once a week with a home-cooked meal.
During life’s difficult moments, the importance of food is often overlooked. Not only is it very hard to find the time or energy to eat, cooking is usually the very last thing to receive attention. When a friend committed to delivering a weekly meal along with his company, it became a true lifeline for our family.
4. I’m organizing a meal drop off this month with a group of friends.
When another good friend asked if she could organize our common friends to drop off home-cooked meals every Tuesday and Thursday for a month, I agreed. Sharing the cooking as a group fostered a sense of community and my family felt so uplifted by our friend’s goodwill. Because our daughter’s chemotherapy treatment spanned a long period of time, friends let us decide if the meal plan was still helpful at the end of every month.
Over time, other friends experienced their own roadblocks and among our group, the tradition of a cooking tree has served us well. I’ve now been on both the giving and receiving side of meal delivery and cannot believe how touching the practice is.
5. I am coming to visit.
There is nothing like the physical presence of a good friend amidst a crisis. When a good friend can be a witness, hold your hand, dry tears, ask how you are feeling in this moment, all of this helps on the journey towards healing. When an offer to visit at the hospital or at home came up, I never turned it down. It was especially helpful if friends offered a specific window of availability such as two hours in the afternoon on Saturday or Sunday. The more specific the better.
6. I’ve located a support group that might be helpful.
There are many online listservs, hangouts, communities and support groups that focus on a variety of topics. Often in the midst of tragedy, there is little time to reflect on or locate helpful resources. This can lead to feelings of being overwhelmed or isolated. Connecting with others that are going through the same thing often provides insight and relief from suffering.
One friend located and suggested I join a cancer support group on Facebook that focused on the very specific kind of childhood cancer my daughter had been diagnosed with and while I initially hesitated because I thought it would clog up my feed, I now find the updates informative and it has also led to new friendships and a sense of shared humanity.
7. I will help with fundraising.
Illness, death and other tragedies often incur unanticipated expenses. When a friend offered to help set up a fundraising site for my daughter, and another spread the word about it, the tender messages and generous donations that came in through the site moved us tremendously and were so practical in helping us face the mounting expenses of travel and medical bills. There are now so many wonderful websites that enable point-and-click fundraising for a loved one in need.
8. You are constantly in my thoughts.
When a friend offers positive, healing thoughts, it is a caring, supportive act that can transcend spiritual affiliation. I’ve had friends put my daughter’s name on Tibetan prayer wheels, lift our family up through Christian prayer groups, speak of her health in both Jewish and Muslim religious ceremonies, and even send Reiki distant energy healing. I’ve always welcomed all good-intentioned, positive thoughts.
At my lowest points, whenever I received a spontaneous text or email that informed me we were in a friend’s thoughts at that very moment, it was incredibly moving.
9. Is there an opportunity to celebrate?
There may be an opportunity, when some time has passed and bad news is not so fresh, to recall a positive memory or mark an occasion related to the situation. I received a small handmade book of photo memories from birth through year four on the occasion of my daughter’s 4th birthday. Receiving this thoughtful collection of photos amidst her health crisis, reminded us of happy times. In addition to her birthday, we also managed to mark Halloween by celebrating ancestors that passed before us and Thanksgiving by incorporating a daily recording of what we were grateful for during the month of November.
While I did not feel as celebratory or festive during these events as in past years, going through the familiar motions and traditions encouraged hopefulness within that we would get through this.
10. You are amazing. You are so strong. You will get through this.
A positive affirmation is often the most straightforward way to offer support. Don’t hesitate to remind your friend how resilient she is. Frequently repeat a sentiment that you sincerely believe and soon your friend will also believe those words. Remind her that while it may be a difficult year ahead, she will get through it because she is strong. She is amazing. And she will be even stronger after persevering through the experience.
When responding to bad news, do not put the onus on the person enduring the hardship to tell you what you can do to help. These recommendations are all examples of effective words and actionable items that will allow you to contribute. Try one of these ten recommendations the next time someone needs you to be there in a meaningful way.
Sky Khan is a founding member of the New York Zen Center for Contemplative Care and an active presence at the Haven Hospice in New York City’s Bellevue Hospital where she provides compassionate care for the terminally ill and dying. She is the founder of Generous.nyc and a speaker, author and educator on the topic of generosity. She is also an advisor to cancerversary.nyc, zenyc.org and grief.nyc.
Heri’s Health Points: Why a good sleep should be your priority
When improving wellness, better sleep should a priority vs nutrition, fitness programs or prescription

Too often, the focus is on being more active, look into new diets or exotic holidays.
These would bring energy, improve strength or cure depression.
The cornerstone of a sustainable and healthy body is quality sleep.
Many brush off sleep. Society or human groups do not value or celebrate when you take a good night sleep. Nobody gets alarmed when you miss a night sleep. Even, all-nighters marathons are celebrated as a proof of motivation and dedication.
Yet, lack of sleep or sleep deprivation deregulates main body functions : impaired brain activity, cognitive dysfunction, weakened immune response, hormonal system dysfunction, poor muscle repair, risk of Type 2 diabetes, higher blood pressure, weight gain, heart disease and so on.
This means quality sleep must be a priority, above nutrition, leisure, physical activity and even work.
Here’s my sleeping plan, let me know if it is good for you:
- If I do not feel well, I try to see first if I had quality sleep recently, before thinking of stress, nutrition or anything else.
- I close negative emotions.
- If I have not been sleeping well recently, I make sure not to overstrain. That means in order : not taking any caffeine (coffee or tea) 5 hours before sleep, no strenuous exercise, no blue light 3 hours before sleep, lower home temperature 2 hours before sleep, massage 1 hour before sleep, camomille tisane 1 hour before sleep.
- Moderate exercise such as 30mn walking at a good pace at 5pm can improve sleep.
- Move or change sleeping conditions if not optimal. That can include moving out or thinking about the sound environment.
- Activity trackers and sleep apps can help measure good sleep and give insights. However, trackers do not improve sleep quality and impact is limited.
References:
- D. J. Bartlett, N. S. Marshall, A. Williams, R. R. Grunstein. June 2007. Sleep health New South Wales: chronic sleep restriction and daytime sleepiness. Internal Medecine Journal
- June J. Pilcher PhD & Elizabeth S. Ott BS. March 2010. Relationships Between Sleep and Measures of Health and Weil-Being in College Students: A Repeated Measures Approach. Journal of Behavioral Medecine.
- Hideki Tanaka, Shuichiro Shirakawa. May 2004. Sleep health, lifestyle and mental health in the Japanese elderly. Journal of Psychomatic Research
- Making sleep a priority – Daily Health Points
Menu
Want to feel better? Write down your thoughts and then decide what to do with them.

In experiments with students it has been found that writing down your thoughts, in your own handwriting, can help you feel more positive, provided you fling away your negative ruminations and keep your positive ones close.
Professor Richard Petty of Ohio State University Psychology department collaborated with colleagues in Spain and tested 83 high school students.
Spending time looking at your negative thoughts make you feel bad about yourself. Throwing out negative and positive thoughts immediately has little impact on you, but putting your positive thoughts in your pocket or purse and referring to them later, has all round positive effects on your mood and future behaviour.
Computerised lists that were either retained or deleted had some effect too, but simply imagining that you had deleted them didn’t work.
(Reported in Human Givens Volume 1 2013 from Brinol P et al, Treating thoughts as material objects can increase or decrease their impact on evaluation. Psychological Science, 24, 1, 41-7)
My comments: this little tip could be very helpful. I know that people who keep journals tend to be more depressed than average. This could be partly due to the introspective nature of journal writing but also perhaps because negative thoughts or events can be reinforced by referring to them or even just carrying them around!
For avid diary writers perhaps they should keep two journals, one only keep the good events thoughts and another much smaller book that can be thrown in the trash every so often, preferably quite frequently.
It could also help when you want to achieve something. Put all of the pros in one list, all the cons on the other, and simply toss out the cons!
Limited time to exercise? Weekend warriors still benefit

From BMJ 14th January 2017
Although guidelines recommend spreading exercise throughout the week, weekend warriors, who compress the recommended amount into the weekend, still experience substantial benefits.
JAMA Internal Medicine reported that risk of death from all causes were 30% down, cardiovascular disease deaths were 40% down and cancer deaths were 18% down, compared to inactive adults.
(doi:10.1136/bmj.j126)
Jovina cooks Italian: Sea bass Genoa Style
Cooking the Italian Provinces – Genova | jovinacooksitalian
Sea Bass Genoa Style
Ingredients
2 pounds Yukon Gold potatoes, peeled and sliced 1/2 inch thick (omit if you are low carbing)
1 pound tomatoes, cut into large chunks
3/4 cup pitted green olives
1/4 cup torn basil leaves
1/2 cup plus 3 tablespoons extra-virgin olive oil
Salt and freshly ground pepper
Two 3-pound whole sea bass or red snapper, or cut into fillets
1/2 cup pine nuts
Directions
Preheat the oven to 425° F. In a very large roasting pan, toss the potatoes, tomatoes, olives and basil with 1/2 cup of the olive oil. Season with salt and pepper.
Rub each fish or the fillets with the 3 tablespoons of olive oil and season with salt and pepper. Set the fish in the roasting pan with the vegetables. Roast for about 30 minutes for the fillets or 40 minutes for the whole fish, until the vegetables are tender and the fish are cooked through.
Meanwhile, in a small skillet, toast the pine nuts over moderate heat, stirring, until golden, about 3 minutes. Spoon the pine nuts over the fish and vegetables in the roasting pan and serve right away.
BMJ stands by Nina Teicholz despite demands for a retraction
 Feature Nutrition
Feature Nutrition
The scientific report guiding the US dietary guidelines: is it scientific?
BMJ 2015; 351 doi: http://dx.doi.org/10.1136/bmj.h4962 (Published 23 September 2015) Cite this as: BMJ 2015;351:h4962
Response by Nina Teicholz
Primary Care Women’s Health Forum: Ten tips for Polycystic Ovary Syndrome
The Primary Care Women’s Health Forum offer their best ten tips for helping women with Polycystic Ovary Syndrome.
Consider PCOS in women with no periods or a cycle length over 35 days whatever the woman’s BMI.
Consider PCOS in adult onset acne.
Ultrasound may not be required to make the diagnosis, but if you are doing it transvaginal ultrasound is best.
Lifestyle advice is required for diet and exercise.
Treat hyper-androgenic signs with combined hormonal contraceptives and if there are undue cardiovascular risks refer to a specialist for help.
Psychological symptoms are common. The Verity site: http://www.verity-pcos.org.uk can help.
Normalise BMI and other risk factors before pregnancy.
PCOS is a lifelong condition and needs individualised, holistic care.
Offer endometrial protection to prevent endometrial hyperplasia.
Offer annual screening to reduce risk factors for cardiovascular disease.
Weight loss increases hunger: a major obstacle for maintenance
 We know about the issue of slowed metabolism after weight loss due to the lean muscle mass loss that goes along with fat loss. This is one reason why higher protein/low carb diets work better than low fat diets; because muscle mass is maintained better. Well, new information from Diabetes in Control backs up what some of us know intuitively or may have experienced personally….
We know about the issue of slowed metabolism after weight loss due to the lean muscle mass loss that goes along with fat loss. This is one reason why higher protein/low carb diets work better than low fat diets; because muscle mass is maintained better. Well, new information from Diabetes in Control backs up what some of us know intuitively or may have experienced personally….
Losing Weight Increases Hunger
The study showed that for every kg of weight they lost, patients consumed an extra 100 calories a day — more than three times what they would need to maintain the lower weight.
This out-of-proportion increase in appetite when patients lost a small amount of weight may explain why maintaining long-term reduced body weight is so difficult.
A validated mathematical method was used to calculate energy intake changes during a 52-week placebo-controlled trial in 153 patients treated with canagliflozin, a sodium glucose co-transporter inhibitor that increases urinary glucose excretion, thereby resulting in weight loss without patients being directly aware of the energy deficit. The relationship between the body weight time course and the calculated energy intake changes was analyzed using principles from engineering control theory.
Previous studies show that metabolism slows when patients lose weight; however, these results suggest that proportional increases in appetite likely play an even more important role in weight plateaus and weight regain.
Knowing that patients with type 2 diabetes who receive the sodium-glucose cotransporter 2 (SGLT-2) inhibitor canagliflozin (Invokana) as part of a glucose-lowering strategy excrete a fixed amount of glucose in the urine (which causes weight loss), they used a mathematical model to calculate energy-intake changes during a 52-week placebo-controlled trial of the drug, in which 153 patients received 300-mg/day canagliflozin and 89 patients received placebo. Using this approach meant that the participants who received canagliflozin consistently excreted 90-g/day glucose but were not aware of the energy deficit.
Previously, the researchers had validated a mathematical model to calculate the expected changes in caloric intake corresponding to changes in body weight (Am J Clin Nutr. 2015;102:353-358). They input the current study data into this model.
At study end, the patients who had received placebo had lost less than 1 kg and those who had received canagliflozin had lost about 4 kg. The weight loss with canagliflozin was less than predicted, due to the patients’ increased appetite. On average, patients who received canagliflozin ate about 100 kcal/day more per kg of weight lost — an amount more than threefold larger than the corresponding energy-expenditure adaptations.
“Our results provide the first quantification of the energy-intake feedback-control system in free-living humans,” the researchers write.
They add that in the absence of “ongoing efforts to restrain food intake following weight loss, feedback control of energy intake will result in eating above baseline levels with an accompanying acceleration of weight regain.”
The findings suggest that “a relatively modest increased appetite might explain a lot of the difficulty that people are having in both losing the weight and maintaining that weight loss over time. From the results it was concluded that, while energy expenditure adaptations have often been considered the main reason for slowing of weight loss and subsequent regain, feedback control of energy intake plays an even larger role and helps explain why long-term maintenance of a reduced body weight is so difficult.
The findings suggest that an increased appetite is an even stronger driver of weight regain than slowed metabolism. “The message to clinicians is to not only push physical activity as a way to counter weight regain but also use medications that impact appetite.”
In summary, the researchers conclude the few individuals who successfully maintain weight loss over the long term do so by heroic and vigilant efforts to maintain behavior changes in the face of increased appetite along with persistent suppression of energy expenditure in an omnipresent obesogenic environment. Permanently subverting or countering this feedback control system poses a major challenge for the development of effective obesity therapies.
Practice Pearls:
- Findings suggest that an increased appetite is an even stronger driver of weight regain than slowed metabolism.
- Appetite increased by ∼100 kcal/day above baseline per kilogram of lost weight.
- The message to clinicians is to not only push physical activity as a way to counter weight regain, but also use medications that impact appetite.
Obesity. 2016;24:2289-2295. Abstract











I’m delighted that The BMJ has stood by this article and decided against retraction. Two outside reviewers judged that the criticisms of the piece did not merit its retraction, and in the end, the corrections made by The BMJ do not, in my view, materially undermine any of the article’s key claims. This article therefore stands as one of the most serious ever, peer-reviewed critiques of the expert report for the US Dietary Guidelines for Americans (DGAs).
The importance of the DGAs, and therefore of this article, should not be understated (and indeed was recognized by many in the mainstream media when the article was published). The DGAs have long been considered the “gold standard,” informing the US food supply, military rations, US government feeding assistance programs such as the National School Lunch Program which are, altogether, consumed by 1 in 4 Americans each month, as well as the guidelines of professional societies and governments around the world, and eating habits generally.
Yet rates of obesity began to shoot upwards in the very year, 1980, that the DGAs were introduced, and the diabetes epidemic began soon thereafter. A critically important yet little understood issue is why the DGAs have failed, so spectacularly, to safeguard health from the very nutrition-related diseases that they were supposed to prevent.
In documenting fundamental failures in the science behind the DGAs, this article offers new insights; It establishes that a vast amount of nutrition science funded by the National Institutes of Health and other governments worldwide has, for decades, been systematically ignored or dismissed, and that therefore, that the DGAs are not based on a comprehensive reviews of the most rigorous science. Incorporating this long-ignored relevant science would likely lead to fundamentally different DGAs and could very well be an important step in infusing them with the power to better fight the nutrition-related diseases.
A fundamental question is why 170+ researchers (including all the 2015 DGA committee members, or “DGAC”), organized by the advocacy group, the Center for Science in the Public Interest (CSPI), would sign a letter asking for retraction. After all, in the weeks following publication, any person had the opportunity to submit a “Rapid Response” to the article, and both CSPI and the DGAC did so, alleging many errors. I responded to them all in my Rapid Response. This is the normal post-publication process.
Yet after all this, CSPI returned for a second round of criticisms, recycling two of the issues (CSPI points #3 and #10) that I had already addressed in my Rapid Response (and which had required no correction), adding another 9 (one of which, #4, contained no challenge of fact), and demanding that based on these alleged errors, the article be retracted. CSPI then circulated this letter widely to colleagues and asked them to sign on.
This lack of substance in the retraction effort seems to point to the reality that it was first and foremost an act of advocacy—a heavy handed attempt to silence arguments with which CSPI, a longtime supporter of the Dietary Guidelines and its allies disagree.[ footnote 1] And this applies not just to the retraction letter but to other CSPI efforts to stifle alternative viewpoints. Earlier this year, for example, I was dis-invited from the National Food Policy Conference after CSPI, together with the USDA official in charge of the Dietary Guidelines, threatened to withdraw if I were included, details of which are reported here and which a Spiked columnist called an act of “censorship.”
It’s important to note that I am not the only person disturbed by the lack of rigorous science underpinning our dietary guidelines. Numerous scientists around the world have expressed concern about the science. And indeed, this consternation is shared by no less than the US Congress, which held a hearing on Oct 7, 2015 to address its serious doubts about the DGAs. Such was this concern that last year that Congress mandated the first-ever major peer-review of the DGAs, by the National Academy of Medicine. Congress appropriated $1 million for this review, and it additionally stipulated that all members of the 2015 DGA committee recuse themselves from the process.
What is the dangerous information challenging the DGAs that cannot be heard on a conference panel nor published in a peer-reviewed journal?
The major findings of this article are that:
1. The DGAC’s finding that the evidence of a “strong” link between saturated fats and heart disease was not clearly supported by the evidence cited. (Note that as of last year, the Heart and Stroke Foundation of Canada no longer limits saturated fats. Note, also, that Frank Hu, the Harvard epidemiologist in charge of the DGAC review on saturated fats, was an energetic promoter of the retraction letter against my article that critiqued his review, according to emails obtained through FOIA requests);
2. Successive DGA committees have for decades ignored or dismissed a large body of rigorous (randomized controlled trial) literature on the low-fat diet, on more than 50K subjects, collectively finding that this diet is ineffective for fighting obesity, diabetes, heart disease or any kind of cancer;
3. Although the DGAs have for decades recommended avoiding saturated fats and cholesterol to prevent heart disease, no DGA committee has ever directly reviewed the enormous body of rigorous (government-funded, randomized controlled trials) evidence, testing more than 25,000 people, on this hypothesis. Many reviews of this data have concluded that saturated fats have no effect on cardiovascular mortality;
4. The DGAC ignored a large body of scientific literature on low-carbohydrate diets (including several “long term” trials, of 2-years duration) demonstrating that these diets are safe and highly effective for combatting obesity, diabetes, and heart disease;
5. The Nutrition Evidence Library (NEL) set up by USDA to do systematic reviews of the science did not meet its own standards for its review of saturated fats in 2010;
6. Although the DGAC is supposed to consult the NEL to conduct systematic reviews of the science, the 2015 DGAC did so for only 67% of the questions that required systematic reviews;
7. For a number of key reviews, the 2015 DGAC relied on work done in part by the American Heart Association and the American College of Cardiology, which are private associations supported by industry and therefore have a potential conflict of interest;
8. The DGAs, for the first time, introduce the “vegetarian diet” as one of its three, recommended “Dietary Patterns,” yet a NEL review of this diet concluded that the evidence for this its disease-fighting powers is only “limited,” which is the lowest rank of evidence assigned for available data;
9. The DGA’s three recommended “Dietary Patterns” are supported by only limited evidence. The NEL review found only “limited” or “insufficient” evidence that the diets could combat diabetes and only “moderate” evidence that the diets can help people lose weight. The report also gave a strong rating to the evidence that its recommended diets can fight heart disease, yet here, several studies are presented, but none unambiguously supports this claim. In conclusion, the quantity of recommended diets are supported by a small quantity of rigorous evidence that only marginally supports claims that these diets can promote better health than alternatives;
10. The DGA process does not require committee members to disclose conflicts of interest and also that, for the first time, the committee chair came not from a university but from industry;
11. The 2015 DGAC conducted a number of reviews in ways that were not systematic. This allowed for the potential introduction of bias (e.g., cherry picking of the evidence).
This last claim, on the systematic nature of the DGAC reviews, is the subject of the corrections published in The BMJ this week, and refer to CSPI points #1, #2, #7, and #8 (two of which are statements in the text and two of which are in the supporting tables). I am grateful to have had the opportunity to work with The BMJ on developing this notice.
The BMJ has placed a word limit on my response. For the rest of this comment, please see: http://thebigfatsurprise.com/comment-bmj-correction-notice/
Footnote 1
CSPI has fought for decades to eliminate saturated fats from the American food supply (so much so, that throughout the late 1980s, CSPI advocated for replacing saturated fats with trans fats and succeeded in driving up consumption of trans fats to historic levels, as described in The Big Fat Surprise, pp.227-228). CSPI has also long advocated for shifting away from animal foods containing saturated fats, towards a plant-based diet based on grains and industrial vegetable oils. The researchers who joined CSPI in signing the letter are largely adherents to this view; many have participated in generating the science that has been used to support the hypothesis that fat and cholesterol cause heart disease, and it is upon this hypothesis that the Guidelines have been based.
Competing interests: I have read and understood BMJ policy on declaration of interests and declare that I am the author of The Big Fat Surprise (Simon & Schuster, 2014), on the history, science, and politics of dietary fat recommendations. I have received modest honorariums for presenting my research findings presented in the book to a variety of groups related to the medical, restaurant, financial, meat, and dairy industries. I am also a board member of a non-profit organization, the Nutrition Coalition, dedicated to ensuring that nutrition policy is based on rigorous science.