
For many years, I have focused on aspects of lifestyle and health management that can enhance quality of life, especially when living with a chronic disease like diabetes, rather than simply on living a long time (longevity). Much of my motivation is derived from the personal experience of watching my maternal grandmother suffer through six (long) years of severe disability related to cardiovascular complications of diabetes starting at the age of 70 that left her unable to feed herself or communicate, bed bound, and with almost no quality of life for her final six years of life. Really, what is the point of simply being alive when you’re really not experiencing life under such conditions?
This topic has come up again recently. New research published online ahead of print in Diabetologia in Spring 2016 (1) presented results showing that the life expectancy and disability-free life expectancy (with 95% uncertainty interval) at age 50 years were 30.2 and 12.7 years, respectively, for men with diabetes, and 33.9 and 13.1 years for women with diabetes. Really think about what those estimates mean: If you’re female and have diabetes at age 50, you would be expected to live almost to age 84, but likely be disabled in some way from the age of 71 forward. If the disability is severe (as in the case of my stroked-out grandmother), then that is a lot of pointless years of being alive without really living, not to mention the cost of caring for someone with medical disabilities that could be a huge burden to your family and the health care system.
Admittedly, that’s pretty discouraging. The best solution may be to focus on what we can do to prevent disability as we age rather than simply living longer, especially with diabetes. Here are three proven ways to improve your quality of life with diabetes (and likely your longevity):
1. Exercise regularly and be more physically active overall.
Even if you already have some diabetes-related health issues like peripheral neuropathy, which can negatively impact quality of life, exercising regularly can help. In a small study on older adults with diabetes and neuropathy, engaging in just 8 weeks of moderate-intensity aerobic exercise was shown to be a cornerstone in improving their quality of life, including experiencing less pain, more feeling in their feet, less restriction in their activities of daily living, better social interactions, and a greater overall life quality—just after 8 weeks of training (2). Other types of physical activity have similar and profound effects on living well with neuropathy (3), so choose the activities that you enjoy doing the most and start with those.
2. Eat more fiber, found abundantly naturally in plant-based foods.
We all know we should be eating more fiber, but where can you find it (besides in Metamucil, which may not have the same health benefits)? Look for it in plant-based foods, mainly fruits, vegetables, grains, beans, and nuts and seeds. Why can it enhance your health and quality of life? Dietary fiber and whole grains contain a unique blend of bioactive components including resistant starches, vitamins, minerals, phytochemicals, and antioxidants, all of which are critical to healthy living. A higher fiber intake helps prevent or protect against many of the health issues that can decrease both quality of life and longevity, including certain gastrointestinal diseases, constipation, hemorrhoids, colon cancer, gastroesophageal reflux disease, duodenal ulcer, diverticulitis, obesity, diabetes, stroke, hypertension, and cardiovascular diseases (4). It also keeps the healthful gut bacteria in your digestive tract more abundant, which directly can benefit health and even prevent obesity. Aim for as much as 50 grams of fiber in your daily diet for optimal health.
3. Improve the quality and quantity of your sleep.
Both sleeping better and sleeping adequate amounts (7 to 8 hours a night for most adults) lower insulin resistance and can help improve diabetes control; alternately, not getting enough good sleep can make your blood glucose levels much harder to manage effectively. As you age, it may require taking a melatonin supplement to help you fall asleep and may help improve diabetes control (5), but exercising regularly certainly assists in both as well, so try taking your daily dose of exercise to optimize sleep.
Get started on these three easy changes today to improve your chances for living longer without disabilities. Remember, there’s more to life than living a long time. What’s the point of living longer if you can’t live well and feel your best every day of your life? It really is your choice to make because you can affect the outcome.
References cited:
1.Huo L, et al. “Burden of diabetes in Australia: life expectancy and disability-free life expectancy in adults with diabetes” Diabetologia 2016; DOI: 10.1007/s00125-016-3948-x.
2.Dixit S, Maiya A, Shastry B: Effect of aerobic exercise on quality of life in population with diabetic peripheral neuropathy in type 2 diabetes: a single blind, randomized controlled trial. Quality of Life Research 2014;23:1629-1640
3.Streckmann F, Zopf EM, Lehmann HC, May K, Rizza J, Zimmer P, Gollhofer A, Bloch W, Baumann FT: Exercise intervention studies in patients with peripheral neuropathy: a systematic review. Sports Med 2014;44:1289-1304
4.Otles S, Ozgoz S: Health effects of dietary fiber. Acta Scientiarum Polonorum Technologia Alimentaria 2014;13:191-202
5.Grieco CR, Colberg SR, Somma CT, Thompson A, Vinik AI: Melatonin supplementation lowers oxidative stress and improves glycemic control in type 2 diabetes. International Journal of Diabetes Research, 2(3): 45-49, 2013 (doi: 10.5923/j.diabetes.20130203.02)
In addition to my educational web site, Diabetes Motion (www.diabetesmotion.com), I also recently founded an academy for fitness and other professionals seeking continuing education enabling them to effectively work with people with diabetes and exercise: Diabetes Motion Academy, accessible at http://www.dmacademy.com. Please visit those sites and my personal one (www.shericolberg.com) for more useful information about being active with diabetes.
by Dr. Sheri Colberg, Ph.D., FACSM
Published in Diabetes in Control 2nd July 2016





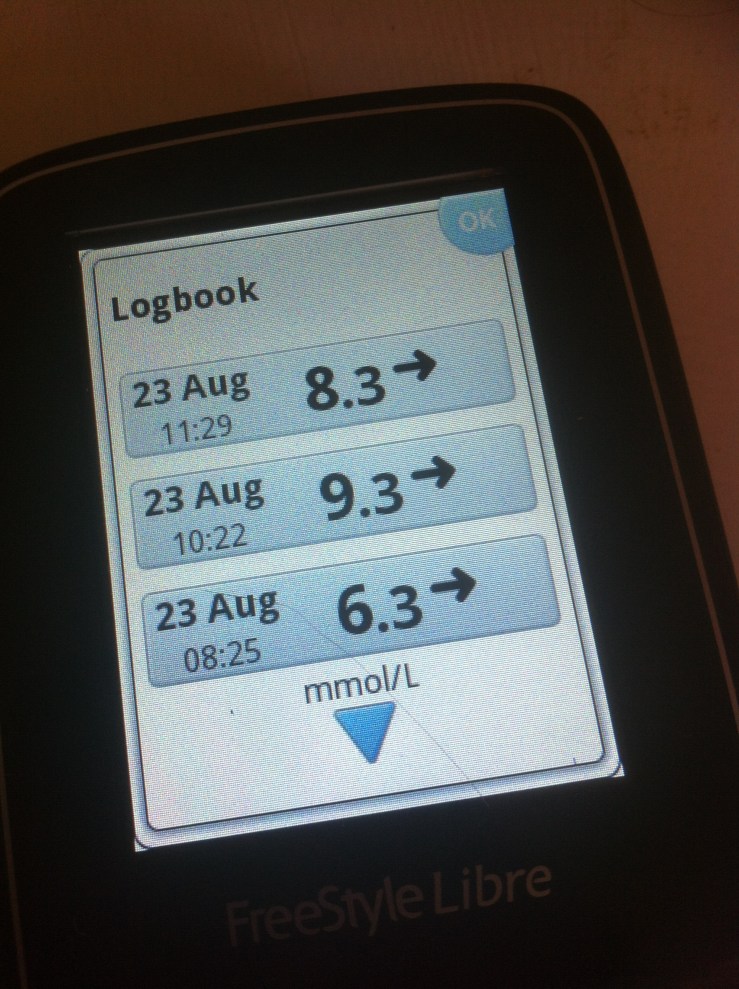 Vancouver doctors took 12 patients type two diabetes who were using insulin and gave them continuous blood sugar monitors to help them improve their blood sugars.
Vancouver doctors took 12 patients type two diabetes who were using insulin and gave them continuous blood sugar monitors to help them improve their blood sugars.










 The USA company Genteel have developed a new lancet device that is reported to be painless and can be used successfully for blood sampling in a variety of sites. It is only available in the USA but can be shipped from there. It does cost $129 plus lancets and postage so it does not come cheap. The manufacturers explained how the new device has a role in diabetes management….
The USA company Genteel have developed a new lancet device that is reported to be painless and can be used successfully for blood sampling in a variety of sites. It is only available in the USA but can be shipped from there. It does cost $129 plus lancets and postage so it does not come cheap. The manufacturers explained how the new device has a role in diabetes management….




