The USA company Genteel have developed a new lancet device that is reported to be painless and can be used successfully for blood sampling in a variety of sites. It is only available in the USA but can be shipped from there. It does cost $129 plus lancets and postage so it does not come cheap. The manufacturers explained how the new device has a role in diabetes management….
The USA company Genteel have developed a new lancet device that is reported to be painless and can be used successfully for blood sampling in a variety of sites. It is only available in the USA but can be shipped from there. It does cost $129 plus lancets and postage so it does not come cheap. The manufacturers explained how the new device has a role in diabetes management….
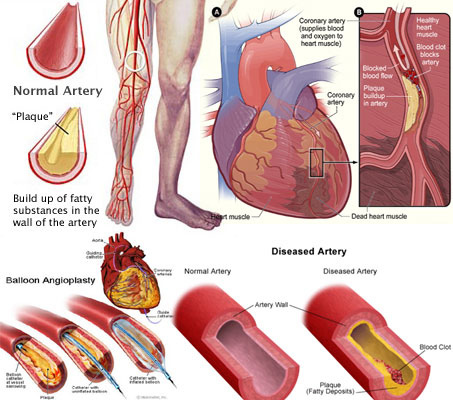
The common belief, presently held by many endocrinologists, is that test blood, drawn from the fingertips, gives a more current and accurate indication of blood glucose than blood drawn from alternate sites, such as the forearm, shoulder and stomach. Unfortunately, for many with diabetes, the fingertip areas are those most laden with pain nerves, causing the lancing process to be the most sensitive and uncomfortable as well as leaving the finger tips bruised, calloused and with reduced tactile sensation.
Fortunately, Genteel researchers have found four new test sites that appear to give the same response time and accuracy as finger tips, now affording the option of relief to these most common testing sites. These two sites are located on the fleshy area of the palms, on a line between where the thumb joins the palm and the center of the wrist (thenar), and fleshy area along a line connecting where the pinky joins the palm to the wrist (hypothenar).

To verify this assertion, the following tests were done at Genteel’s test facility. Test subjects fell into three categories: non-diabetic, pre-diabetic, and under-control diabetic. Tests consisted of simultaneously taking blood samples from alternate sites, such as the forearm, fingertips and from the thenar/hypothenar areas. The tests began at (t=0) after a prolonged period (at least 2 hours, and mostly after arising from a night’s sleep). This was considered the static blood glucose level, or baseline. Before first blood drawn all subjects sat for 15 minutes in a room at a temperature of between 68 and 73°F. At the start time (t=0), each test subject consumed the standard 15-gram load of fast-acting glucose. Thereafter, at 5-minute intervals, blood glucose levels were simultaneously measured in these same three test areas: alternate site, finger tips, and either the thenar or hypthenar areas. After testing at 5-minute intervals for 1 hour, test intervals were increased to 10 minutes, for another hour, or until blood glucose levels returned to at, or near, baseline levels, whichever came first.
Four Charts Using Typical Data, Out of the 24 Subjects Tested
Figure 1.1: Measuring Rate of Change Between Calf/Knee (Alternate Site), Finger Tip, Thenar and Hypothenar Eminence of Palm – #17

Figure 1.2: Measuring Rate of Change Between Calf/Knee (Alternate Site), Finger Tip, Thenar and Hypothenar Eminence of Palm – #31

Figure 1.3: Measuring Rate of Change Between Calf/Knee (Alternate Site), Finger Tip, Thenar and Hypothenar Eminence of Palm – #23

Figure 1.4: Measuring Rate of Change Between Calf/Knee (Alternate Site), Finger Tip, Thenar and Hypothenar Eminence of Palm – #27

Figure 1.5: Measuring Rate of Change Between Calf/Knee (Alternate Site), Finger Tip, Thenar and Hypothenar Eminence of Palm – DG

Conclusion:
Blood glucose levels on the thenar and hypothenar areas of both hands consistency matched those on the finger tips well within meter accuracy. Both areas had matching bell shaped curves reaching approximately (within meter accuracy) the same growth rates and peak levels at the same times. The alternate site not only lagged behind both the thenar and hypothenar areas by about 22 minutes, but only reached about 70% the rise from the static level to peak values.
Genteel’s test lab results indicate that the thenar and hypothenar areas are viable alternatives to finger sticks because they have less pain nerve density. However, blood does not rise easily or readily to the surface in these areas without using specific technology currently present in Genteel’s lancing instrument, and applied over the lancing site. With this technology, comfortable and extremely accurate blood draw is readily available, allowing finger tips to heal and regain sensation.
Contraindications:
All who now wish to test from these new sites should check with their doctor to be certain there are no special metabolic considerations that would preclude you from testing on these new areas.
Literature and laboratory research are continuing on the subject. If you would like to be informed of the latest results, go to support@mygenteel.com, provide your email and add the note, “Palm Research Results.”