
Potato-rich diet ‘may increase pregnancy diabetes risk’
- Eating potatoes or chips on most days of the week may increase a woman’s risk of diabetes during pregnancy, say US researchers.
This is probably because starch in spuds can trigger a sharp rise in blood sugar levels, they say.
Their study in the BMJ tracked more than 21,000 pregnancies.
But UK experts say proof is lacking and lots of people need to eat more starchy foods for fibre, as well as fresh fruit and veg.
The BMJ study linked high potato consumption to a higher diabetes risk.
Swapping a couple of servings a week for other vegetables should counter this, say the authors.
UK dietary advice says starchy foods (carbohydrates) such as potatoes should make up about a third of the food people eat.
There is no official limit on how much carbohydrate people should consume each week.
Starchy carbs
Foods that contain carbohydrates affect blood sugar.
Some – high Glycaemic Index (GI) foods – release the sugar quickly into the bloodstream.
Others – low GI foods – release them more steadily.
Research suggests eating a low GI diet can help manage diabetes.
Pregnancy puts extra demands on the body, and some women develop diabetes at this time.
Gestational diabetes, as it is called, usually goes away after the birth but can pose long-term health risks for the mother and baby.
The BMJ study set out investigate what might make some women more prone to pregnancy diabetes.
The study followed nurses who became pregnant between 1991 and 2001. None of them had any chronic diseases before pregnancy.
What is gestational diabetes mellitus?
- It is a condition where there is too much glucose (sugar) in the blood
- About three in every 100 pregnancies are affected in the UK
- Symptoms include a dry mouth, tiredness and urinating frequently
- Gestational diabetes can be controlled with diet and exercise, but some women will need medication to keep their blood glucose levels under control
- If not managed properly, it could lead to premature birth or miscarriage
Every four years, the women were asked to provide information on how often potatoes featured in their diets, and any cases of gestational diabetes were noted.
Over the 10-year period, there were 21,693 pregnancies and 854 of these were affected by gestational diabetes.
The study took into account other risk factors, such as:
- age
- a family history of diabetes
- overall diet
- physical activity
- obesity
It found a 27% increased risk of diabetes during pregnancy in the nurses who typically ate two to four 100g (3.5oz) servings of boiled, mashed, baked potatoes or chips a week.
In those who ate more than five portions of potatoes or chips a week, the risk went up by 50%.
The researchers estimate that if women swap their potatoes for vegetables or whole grains at least twice a week, they would lower their diabetes risk by 9-12%.
Cuilin Zhang, lead study author, from the National Institutes of Health in Maryland, US, said the findings were important.
“Gestational diabetes can mean women develop pre-eclampsia during pregnancy and hypertension,” she said.
“This can adversely affect the foetus, and in the long term the mother may be at high risk of type-2 diabetes.”
But UK experts stressed there was not enough evidence to warn women off eating lots of potatoes.
Simple swaps that can lower GI
Switch baked or mashed potato for sweet potato or boiled new potatoes
- Instead of white and wholemeal bread, choose granary, pumpernickel or rye bread
- Swap frozen microwaveable French fries for pasta or noodles
- Try porridge, natural muesli or wholegrain breakfast cereals
Dr Emily Burns, of Diabetes UK, said: “This study does not prove that eating potatoes before pregnancy will increase a woman’s risk developing gestational diabetes, but it does highlight a potential association between the two.
“However, as the researchers acknowledge, these results need to be investigated in a controlled trial setting before we can know more.
“What we do know is that women can significantly reduce their risk of developing gestational diabetes by managing their weight through eating a healthy, balanced diet and keeping active.”
Dr Louis Levy, head of nutrition science at Public Health England, said: “As the authors acknowledge, it is not possible to show cause and effect from this study.
“The evidence tells us that we need to eat more starchy foods, such as potatoes, bread, pasta and rice, as well as fruit and vegetables to increase fibre consumption and protect bowel health.
“Our advice remains the same: base meals around a variety of starchy foods, including potatoes with the skin on, and choose wholegrain varieties where possible.”
This is an article published today BBC News
Gestational diabetes – NHS Choices
BMJ – British Medical Journal
Diabetes UK




 about 25 percent of obese people do not have metabolic complications,” he added. “Our data shows that these people remain metabolically normal even after they gain additional weight.”
about 25 percent of obese people do not have metabolic complications,” he added. “Our data shows that these people remain metabolically normal even after they gain additional weight.”
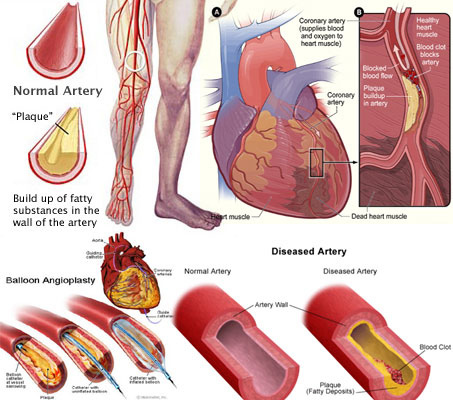
 Over the years, physicians and researchers have advocated less salt consumption in heart failure patients. Although doctors make this recommendation frequently, patients are not always compliant. Heart failure patients who may also be hypertension patients inspired the DASH diet, which includes decreased to no sodium intake, more fruits and vegetables, skinless poultry, and less saturated and trans fat. In heart failure patients, salt increases water retention, which is quite harmful to the function of the heart.
Over the years, physicians and researchers have advocated less salt consumption in heart failure patients. Although doctors make this recommendation frequently, patients are not always compliant. Heart failure patients who may also be hypertension patients inspired the DASH diet, which includes decreased to no sodium intake, more fruits and vegetables, skinless poultry, and less saturated and trans fat. In heart failure patients, salt increases water retention, which is quite harmful to the function of the heart.




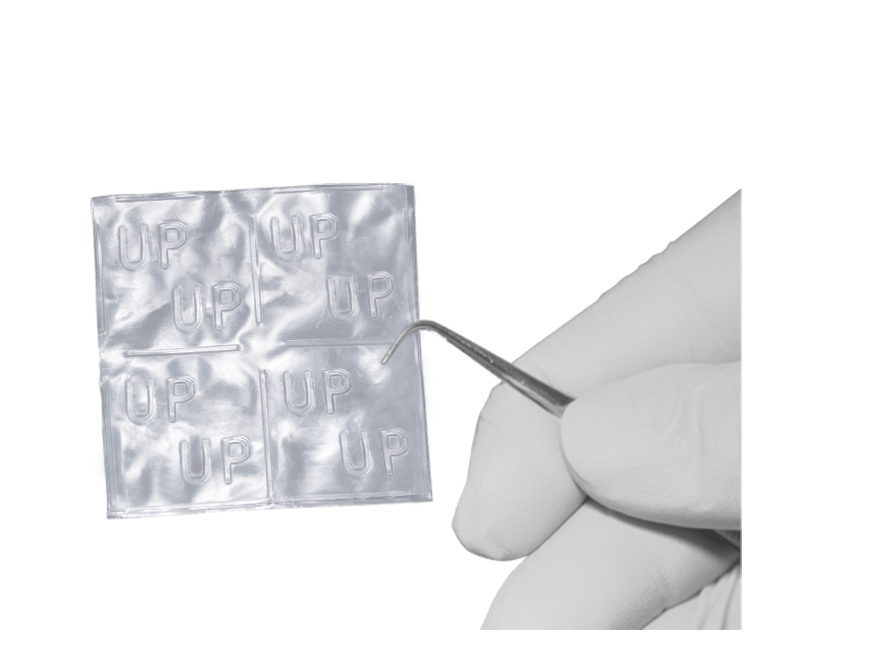
 Diabetic foot ulcers that don’t respond to usual care can respond very well to a new membranous patch that is available to patients in the USA.
Diabetic foot ulcers that don’t respond to usual care can respond very well to a new membranous patch that is available to patients in the USA.

