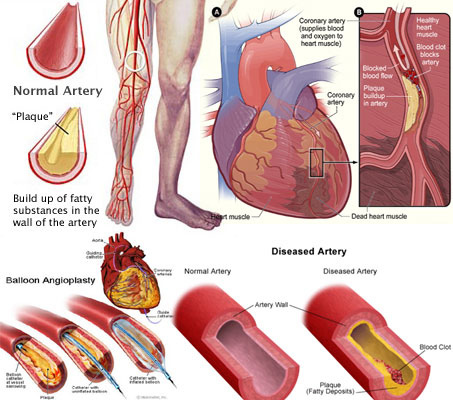
Obesity does not always go hand in hand with metabolic changes in the body that can lead to diabetes, heart disease and stroke, according to a new published study…
In a study at Washington University School of Medicine, researchers found that a subset of obese people do not have common metabolic abnormalities associated with obesity, such as insulin resistance, abnormal blood lipids (high triglycerides and low HDL cholesterol), high blood pressure and excess liver fat.
In addition, obese people who didn’t have these metabolic problems when the study began did not develop them even after they gained more weight.
The study involved 20 obese participants who were asked to gain about 15 pounds over several months to determine how the extra pounds affected their metabolic functions.
First author Elisa Fabbrini, MD, PhD, assistant professor of medicine, added that, “Our goal was to have research participants consume 1,000 extra calories every day until each gained 6 percent of his or her body weight” “This was not easy to do. It is just as difficult to get people to gain weight as it is to get them to lose weight.”
All of the subjects gained weight by eating at fast-food restaurants, under the supervision of a dietitian. The researchers chose fast-food chain restaurants that provide rigorously regulated portion sizes and nutritional information.
Before and after weight gain, the researchers carefully evaluated each study subject’s body composition, insulin sensitivity and ability to regulate blood sugar, liver fat and other measures of metabolic health.
After gaining weight, the metabolic profiles of obese subjects remained normal if they were in the normal range when the study began. But the metabolic profiles significantly worsened after weight gain in obese subjects whose metabolic profiles already were abnormal when the study got underway.
Senior investigator Samuel Klein, MD, the Danforth Professor of Medicine and Nutritional demonstrated that some obese people are protected from the adverse metabolic effects of moderate weight gain, whereas others are predisposed to develop these problems.”
“This observation is important clinically because  about 25 percent of obese people do not have metabolic complications,” he added. “Our data shows that these people remain metabolically normal even after they gain additional weight.”
about 25 percent of obese people do not have metabolic complications,” he added. “Our data shows that these people remain metabolically normal even after they gain additional weight.”
As part of the study, the researchers then helped the subjects lose the weight they had gained.
The researchers identified some key measurements that distinguished metabolically normal obese subjects from those with problems. One was the presence of fat inside the liver. Those with abnormal metabolism accumulated fat there.
Another difference involved gene function in fat tissue. People with normal metabolism in spite of their obesity expressed more genes that regulate fat production and accumulation. And the activity of those genes increased even more when the metabolically normal people gained weight. That wasn’t true for people with abnormal metabolism.
“These results suggest that the ability of body fat to expand and increase in a healthy way may protect some people from the metabolic problems associated with obesity and weight gain.” He noted that obesity contributes to more than 60 different unhealthy conditions.
Practice Pearls:
- Some obese people are protected from the adverse metabolic effects of moderate weight gain.
- Some key measurements that distinguished metabolically normal obese subjects from those with problems. One was the presence of fat inside the liver. Those with abnormal metabolism accumulated fat there.
- People with normal metabolism in spite of their obesity expressed more genes that regulate fat production and accumulation.
Elisa Fabbrini. Metabolically normal obese people are protected from adverse effects following weight gain, pub Jan. 2, 2014 in The Journal of Clinical Investigation. (Published in Diabetes in Control Jan 15)












 about 25 percent of obese people do not have metabolic complications,” he added. “Our data shows that these people remain metabolically normal even after they gain additional weight.”
about 25 percent of obese people do not have metabolic complications,” he added. “Our data shows that these people remain metabolically normal even after they gain additional weight.”