The 2015 Footcare guidelines are forward thinking, evidenced based and if implemented widely should help reduce amputations in diabetics. The problem is that at the moment best possible practice is not happening in many areas including my own.
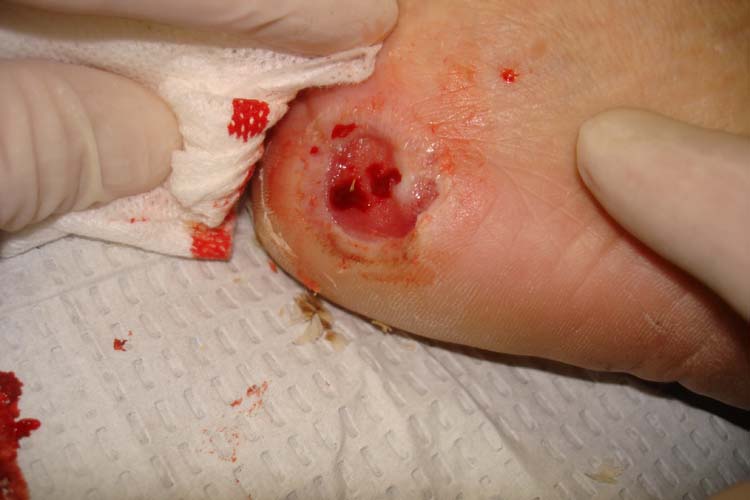
For instance, NICE states that diabetic patients should get information that includes: a clear explanation of their problem, pictures of diabetic foot problems, care of the other foot or leg, foot emergencies and who to contact, footwear advice, wound care, and last but not least, information about diabetes and the importance of blood sugar control. (4.2)
They need this because life expectancy for diabetics is up to 15 years shorter than for their non-diabetic counterparts and 75% of them will die of macrovascular complications. 10% of diabetics will get a foot ulcer at some point in their lives.(1.1)
For every £150 spent on total NHS expenditure £1 is spent dealing with ulcers and amputations. (1.2 2012). Diabetes is the most common cause of non-traumatic amputations and ulcers precede 80% of these. 70% of people die within 5 years of amputation.
The number of amputations for diabetics ranges 4 fold for various reasons across the UK.(1.3) With evidence for best practice available the 2015 guidelines hope to bring poorer performing areas into line. Preventing ulcers and amputations would be very worthwhile not just for the individuals concerned but for the sheer cost of them.
To enable the best possible care NICE recommends that a diabetic foot protection and treatment service is available in the community and in hospitals. (2.3)
The team should include:
Diabetology
Podiatry
Diabetes specialist nurses
Vascular surgery
Microbiology
Orthopaedic surgery
Othotics/biomechanics
Interventional radiology
Casting
Tissue viability
NICE recommends that those with active diabetic foot problems are referred to the foot protection service and that referrals within 24 hours be made for grangrene, suspicion of Charcot’s arthropathy, ulceration with limb ischaemia, clinical concern that there is a deep seated soft tissue or bone infection, ulceration with fever or any signs of bone sepsis. (2.2)
NICE recognises that special arrangements for the housebound, those in nursing homes or in care may need to be made. (2.3)
They also warn that ankle/ brachial pressure index results may need to be interpreted carefully in diabetics because calcified arteries may falsely elevate results and so give falsely reassuring readings. (2.3)
Health care professionals should also know that there is a raised cardiac risk in those with diabetic foot problems. (4.2)
Once a diabetic foot problem is recognised clinically X rays and MRIs may be needed for further investigation. (6.1)
For mild infections antibiotics that cover gram positive organisms should be given. (6.2) This could be for instance flucloxacillin. For severe infections both gram positive and negative organisms should be covered. This would require the addition of eg metronidazole. For severe infections they recommend that IV antibiotics are started first and the switch to oral antibiotics should be based on the clinical response. For those with bone infection the course should be for six weeks.
Charcot’s arthropathy occurs more commonly in those with neuropathy and renal failure. (7.1). Suspect this if there is a red, warm, swollen foot with deformity, even if pain is not reported. Refer this condition urgently and keep the person off the foot. X ray first of all and if no abnormalities are seen do an MRI.
When making a decision on the frequency of follow up for patients with diabetic foot problems, take into account their overall health, how healing has progressed or any deterioration. (4.8). Ensure that the monitoring interval is maintained in the community or in the hospital.
I know that in Ayrshire where I practise there is no such entity as a diabetic foot protection or treatment service although the services are available separately, and I would be interested to know how it is in your areas. The information to diabetics is certainly not as comprehensive as NICE would like. I can see the importance of this because of the need for urgent assessment and treatment of minor problems so that they don’t become limb threatening.
As a GP the main thing I need to do is to recognise diabetic foot problems. If the problem is mild I would treat and review promptly but for severe problems hospital admission is needed. After all most cases will require X rays, MRIs and intravenous antibiotics. There is not the seamless service for diabetics inside and outside of hospital that NICE has found makes such a difference to amputation rates.
For the best advice on caring for your feet if you have diabetes I would recommend Dr Bernstein’s Diabetes Solution. At the present time I don’t know of any good photographic sites that would provide the pictures that would help diabetics understand their foot issues. Any suggestions from our readers?