Susan Pierce Thompson PhD is a neuroscientist who used to be pretty hefty in her teens and twenties till she went on a 12 step programme along the lines of alcoholics anonymous but dealing with the issue of food addiction. She has stayed very slim for the last 12 years and reckons she knows what keeps us from losing weight and keeping it off long term. Indeed she teaches about this subject at university and has recently started online classes with team support to help the food addicts get “happy, thin and free”. She calls her programme Bright Line Eating.
The basics of this is that the “everything in moderation” mantra does not work with the seriously addicted food addict. Flour, sugar and anything that even tastes sweet gets the heave-ho permanently. Could you do this? Of course you could, if you want to get thin and stay thin. But Susan recognises that breaking your intentions happens and that the most important thing is to resume your plan immediately rather than beat yourself up about it, or use a minor deviation as an excuse to binge with a vow to start on Monday again.
Rats as well as humans seem to fall into three groups. The ones who seem able to resist temptation without a problem, the ones who can resist it for a while but then will give in, particularly if under some sort of stress, and the highly addicted who just can’t leave sugar, sweet stuff, refined flour products and white potatoes in all their forms alone. Susan says that modern foods and patterns of eating have hijacked the brain and sap willpower, induce cravings and set up feelings of hunger. Indeed she has found that rats rate sugar water as more pleasurable than cocaine even when they had been made into serious cocaine addicts by researchers.
The taste of anything sweet seems to be a problem. Saccharine, and all artificial sweeteners have the ability to induce cravings, even stevia. Although fat and salt make food more palatable, and humans eat more of it when laced with butter, cream, olive oil and salt for instance, they don’t set up the same addiction circuits. It is the flour/sugar items such as chocolate, ice cream and pizza that are the top addictive foods for most westernised humans, with potatoes and potato products coming in fourth.
When you get a craving for something, parts of your brain are being affected by chemicals that you have no control over. Cravings and hunger are controlled by the hypothalamus. This is your body’s thermostat that controls all sorts of complex processes through the release of hormones.
Your willpower centre is in the anterior cingulate cortex and behaviour is controlled here. The problem is that behaviour gets more difficult to control if you have to withstand temptation for just 15 minutes. It gets even harder to control behaviour when the blood sugar is low or you are already tired, have already had your temptation tested, are feeling emotional or have been focussing on tasks. Susan calls this the “willpower gap”. You know what you are meant to do but you just can’t seem to help yourself from doing something else. Like opening that packet of biscuits.
Your brainstem is where leptin is active. Your brainstem is the most primitive part of the brain and the most basic functions that keep you alive such as breathing reside here. The trouble is that insulin resistance leads to leptin resistance, and although your brain stem may be flooded with leptin, telling you that you are full, the leptin resistance means that the message doesn’t get through, and your brain stem thinks you are starving. Mindless eating ensues just as mindless breathing continues.
A major step in resolving this impasse is that insulin levels need to be lowered. And what raises insulin the most? Yes, sugar and starch. This is why a low carb diet, as we describe in our book, can help you lose weight and get your appetite under control. It is all down to physiology.
Susan goes a bit further than we do, however, in that all sweet stuff, with the exception of sweet fruit, is banned. Also all flour products are completely banned. This is because those people who have very serious food issues are more susceptible to dopamine, the reward hormone.
Dopamine is active in the nucleus accumbens. It goes up in response not only to food stimuli but also to sex stimuli for example. Indeed Susan describes sugar as the pornography equivalent of sex. I have to agree with her here.
In large magazine shops you often see rows of women’s magazines on one side and men’s magazines on the other. The men’s magazines seem to be mainly all about becoming more competent in something eg music, muscle building, computer know-how, with some soft pornography thrown in. Women’s magazines have “how to be more nurturing” magazines with pets, home decorating and crafts taking about a quarter of the space. The rest seems evenly split between “how to make lovely food” often featuring beautifully iced sponge cakes with lashings of cream on the one hand, and “how to get thin from not eating beautifully ices sponge cakes with lashings of cream on them”. I’ve often thought of food articles and particularly photographs as being porn for women.
So, back to dopamine. What a great hormone. You have lots of it and you feel like you rule the world. The downside is that your reward feeling gets worn down by the never ending waves of dopamine and you tend to need a bigger fix for the same wonderful feelings over time. Also if dopamine becomes depleted you can feel pretty unhappy and also can need another fix to bring it up. This is a reason why Zyban, the anti-smoking drug can induce suicidal depression.
Zyban, also known as varenicicline, makes the craving for cigarettes stop by blocking dopamine. When you smoke, you don’t get the hit. Instead you think, “This fag is lousy, why the hell am I smoking it?” This makes it somewhat easier to break the smoking habit. The downside is that you can feel lousy about everything. And sometimes the effect is unpredictably tragic.
Despite the common belief that we are in control of our behaviour rather than our brain chemicals, Susan is so convinced of the chemical superiority over willpower, that she builds methods of how to resist the hijack into her diet plan.
Dr Thompson knows that a chemically affected brain really has the belief that the body is starving and that flour and sugar are even more powerfully addictive than heroin or cocaine for about a third of the population. She knows you can’t reason with your brain stem. Instead it reasons with you.
That little voice says, “I deserve that”. “It’s only one time”. “It’s only a little bit.” As more and more exceptions to our dietary plan creep in, we watch ourselves breaking rules, and the belief that we are incapable and lacking in some way, especially compared to thin people, reduces our feelings of competency. Our self-esteem goes down the plug hole. As I have said before, a prominent bariatric surgeon told me that the drop out rate with bariatric patients was particularly high because of the very low self- esteem that this group of people have.
Susan says that very clear boundaries are necessary to get back on track. A lot of planning, daily preparation, long term habit change and support is necessary to overcome addictive eating. Emergency action plans and support are needed for the inevitable breaks in willpower. But, she says that dopamine receptors recover in time and that as insulin resistance disappears, the insatiable hunger goes with it. She says that reliance on willpower is the single biggest mistake dieters make. Instead you need a whole system to deal with false hunger, addiction and social pressures to eat flour and sugar.
Restorative behaviours such as meditation are important. So is getting out in nature. Anything other than food that boosts your willpower battery is good. Exercise is not part of the plan for most people because it can be a step too far when good eating habits are in the process of being embedded. She thinks exercise can be too much a sap on a person’s willpower unless it is already an entrenched habit.
The path to being slim and healthy is not easy so a different way of looking at the problem is welcome. In particular simple calorie measuring is no good for some people if sugar and flour are part of the calories. Also low carbing may not be extreme enough for some people and cutting out all sweeteners and sugar rather than keeping to small amounts of sugar and starch may be necessary.
Based on an online webinar by Susan Pierce Thompson PhD. October 14 2015.
 An analysis of the ACCORD trial has shown that African Amercans, insulin users, and patients who have episodes of severe hypoglycaemia are at considerably higher risk of running hba1cs over 8%.
An analysis of the ACCORD trial has shown that African Amercans, insulin users, and patients who have episodes of severe hypoglycaemia are at considerably higher risk of running hba1cs over 8%.




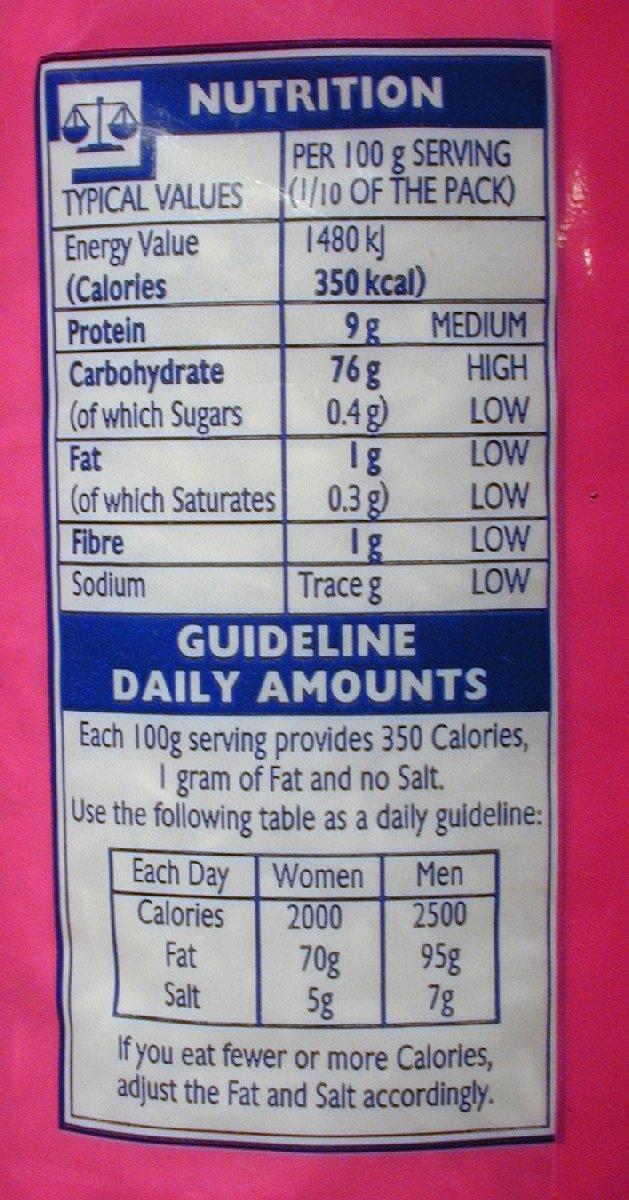
 “A holistic approach is urgently needed in which food companies, consumers and policy makers, instead of working against one another, manage to find mutually beneficial strategies to combat the world’s alarming obesity epidemic,” the researchers concluded.
“A holistic approach is urgently needed in which food companies, consumers and policy makers, instead of working against one another, manage to find mutually beneficial strategies to combat the world’s alarming obesity epidemic,” the researchers concluded.





